

The Guide to Literature Reviews

- What is a Literature Review?
- The Purpose of Literature Reviews
- Guidelines for Writing a Literature Review
- How to Organize a Literature Review?
- Software for Literature Reviews
- Using Artificial Intelligence for Literature Reviews
- How to Conduct a Literature Review?
- Common Mistakes and Pitfalls in a Literature Review
- Methods for Literature Reviews
- What is a Systematic Literature Review?
- What is a Narrative Literature Review?
- What is a Descriptive Literature Review?
- What is a Scoping Literature Review?
- What is a Realist Literature Review?
- What is a Critical Literature Review?
- Meta Analysis vs. Literature Review
- What is an Umbrella Literature Review?
- Differences Between Annotated Bibliographies and Literature Reviews
- Literature Review vs. Theoretical Framework
- How to Write a Literature Review?
- How to Structure a Literature Review?
- How to Make a Cover Page for a Literature Review?
- Importance of a literature review abstract
How to write a literature review abstract?
Key reminders when writing a literature review abstract.
- How to Write a Literature Review Introduction?
- How to Write the Body of a Literature Review?
- How to Write a Literature Review Conclusion?
- How to Make a Literature Review Bibliography?
- How to Format a Literature Review?
- How Long Should a Literature Review Be?
- Examples of Literature Reviews
- How to Present a Literature Review?
- How to Publish a Literature Review?
How to Write a Literature Review Abstract?
A well-crafted abstract is the initial point of contact between your research and its potential audience. It is crucial to present your work in the best possible light. A literature review abstract is a concise summary of the key points and findings of a literature review that is published as a full paper. It serves as a snapshot of the review, providing readers with a quick overview of the research topic , objectives, main findings, and implications .

Unlike the full literature review, the abstract does not delve into detailed analysis or discussion but highlights the most critical aspects. An abstract helps readers decide whether the full article is relevant to their interests and needs by encapsulating the essence of the literature review. A literature review abstract offers a condensed version of the study that helps researchers identify the review's relevance to their work. This is important in academic settings, where individuals often revise numerous journal articles and papers to find pertinent information. A clear and informative abstract saves time and effort.
Here are the steps we recommend when writing abstracts for literature reviews:
Introduce the research topic : Begin by stating the subject of your literature review. Explain its significance and relevance in your field. Provide context that highlights the broader impact and necessity of your review. For example, "This literature review focuses on the impact of climate change on coastal ecosystems and its significance in developing sustainable management strategies."
State objectives : Clearly outline the literature review's main objectives or purposes. Specify what you aim to achieve, such as identifying gaps in the literature, synthesizing existing research, or proposing new directions for future studies. For instance, "This review aims to identify key areas where climate change impacts coastal ecosystems and to propose future research directions."
Summarize key findings : Provide a concise summary of the data collection methods and results. Include primary findings, trends, or insights from your review. Highlight the most important conclusions and previous research contributions, and explain their implications for the field. An example might be, "The review reveals significant changes in species composition due to rising sea temperatures, suggesting the need for adaptive management strategies."

Use clear and concise language : Ensure your abstract covers the main points of your literature review, using straightforward language and avoiding complex terminology or jargon. Write in the third person to maintain objectivity, and structure your abstract logically to improve readability. For example, avoid first-person phrases like "I found that..." and use "The review indicates that..." Keep your abstract concise, typically between 150-250 words. Make it comprehensive, offering a clear view of the review’s scope and significance without overwhelming readers with too much detail. Conciseness is key in abstract writing, as it allows readers to quickly grasp the essence of your review without wading through unnecessary information.
Optimize search engines : Incorporate relevant search terms and phrases to enhance discoverability through search engines. Choose a descriptive title that includes key phrases from your literature review. This makes your work more likely to appear with the search results and makes it more accessible to potential readers. With the example above, a researcher may use keywords like "literature review," "climate change," and "coastal ecosystems" to attract the right audience.
Quality literature reviews start with ATLAS.ti
Make your literature reviews stronger, ATLAS.ti is there for you at every step. See how with a free trial.
When writing your abstract, double-check it covers the critical points of your literature review. This includes the research topic, significance, objectives, data extraction methods, main findings, and implications for additional research. Avoiding ambiguity and complex terminology makes your abstract accessible to a wider audience, including those who may not be specialists in your field. Here are some important tips to keep in mind when writing abstracts:
Avoid using complex terminology or scientific jargon that might confuse readers. A good abstract should be accessible to a broad range of potential readers, including researchers and policymakers.
Avoid using quotations in your abstract; paraphrase the information to maintain clarity and conciseness. Write in the third person to ensure your abstract remains professional and focused.
Choose a descriptive title for your article mentioning key phrases from your literature review. Optimize the title for search engines to enhance its visibility and shareability. A well-crafted title can significantly impact the reach and impact of your research. Incorporating keywords into your title improves search engine optimization (SEO) and attracts readers' attention, making your work more discoverable.

Focus on the most important information, avoiding unnecessary details. Ensure a logical flow of ideas with clear and active language. Each sentence should contribute to explaining your literature review's key points. A well-structured abstract guides readers through your review logically, making it easier to follow and understand. It also leads readers through your review smoothly.
Make sure that your abstract accurately reflects the content of your literature review. Use relevant keywords and phrases to ensure your abstract remains focused and pertinent to your research. Accuracy is vital to maintain the interest of your readers and to guide those who read the full review to find the information they expect.
Proofread your abstract carefully to check for grammatical and typographical errors. Ensure that it is well-structured, polished, and error-free.
A well-written literature review abstract is vital for the effective dissemination of your research. It serves as the first impression of your work which engages readers and provides a succinct overview of your study's significance and findings. You will create an abstract that attracts readers and reaches a broader audience by introducing your topic, stating your objectives, summarizing key findings, and using clear language. Writing clear abstracts enhances the visibility, accessibility, and impact of your literature reviews.

Develop powerful literature reviews with ATLAS.ti
Use our intuitive data analysis platform to make the most of your literature review.
Purdue Online Writing Lab Purdue OWL® College of Liberal Arts
Writing a Literature Review

Welcome to the Purdue OWL
This page is brought to you by the OWL at Purdue University. When printing this page, you must include the entire legal notice.
Copyright ©1995-2018 by The Writing Lab & The OWL at Purdue and Purdue University. All rights reserved. This material may not be published, reproduced, broadcast, rewritten, or redistributed without permission. Use of this site constitutes acceptance of our terms and conditions of fair use.
A literature review is a document or section of a document that collects key sources on a topic and discusses those sources in conversation with each other (also called synthesis ). The lit review is an important genre in many disciplines, not just literature (i.e., the study of works of literature such as novels and plays). When we say “literature review” or refer to “the literature,” we are talking about the research ( scholarship ) in a given field. You will often see the terms “the research,” “the scholarship,” and “the literature” used mostly interchangeably.
Where, when, and why would I write a lit review?
There are a number of different situations where you might write a literature review, each with slightly different expectations; different disciplines, too, have field-specific expectations for what a literature review is and does. For instance, in the humanities, authors might include more overt argumentation and interpretation of source material in their literature reviews, whereas in the sciences, authors are more likely to report study designs and results in their literature reviews; these differences reflect these disciplines’ purposes and conventions in scholarship. You should always look at examples from your own discipline and talk to professors or mentors in your field to be sure you understand your discipline’s conventions, for literature reviews as well as for any other genre.
A literature review can be a part of a research paper or scholarly article, usually falling after the introduction and before the research methods sections. In these cases, the lit review just needs to cover scholarship that is important to the issue you are writing about; sometimes it will also cover key sources that informed your research methodology.
Lit reviews can also be standalone pieces, either as assignments in a class or as publications. In a class, a lit review may be assigned to help students familiarize themselves with a topic and with scholarship in their field, get an idea of the other researchers working on the topic they’re interested in, find gaps in existing research in order to propose new projects, and/or develop a theoretical framework and methodology for later research. As a publication, a lit review usually is meant to help make other scholars’ lives easier by collecting and summarizing, synthesizing, and analyzing existing research on a topic. This can be especially helpful for students or scholars getting into a new research area, or for directing an entire community of scholars toward questions that have not yet been answered.
What are the parts of a lit review?
Most lit reviews use a basic introduction-body-conclusion structure; if your lit review is part of a larger paper, the introduction and conclusion pieces may be just a few sentences while you focus most of your attention on the body. If your lit review is a standalone piece, the introduction and conclusion take up more space and give you a place to discuss your goals, research methods, and conclusions separately from where you discuss the literature itself.
Introduction:
- An introductory paragraph that explains what your working topic and thesis is
- A forecast of key topics or texts that will appear in the review
- Potentially, a description of how you found sources and how you analyzed them for inclusion and discussion in the review (more often found in published, standalone literature reviews than in lit review sections in an article or research paper)
- Summarize and synthesize: Give an overview of the main points of each source and combine them into a coherent whole
- Analyze and interpret: Don’t just paraphrase other researchers – add your own interpretations where possible, discussing the significance of findings in relation to the literature as a whole
- Critically Evaluate: Mention the strengths and weaknesses of your sources
- Write in well-structured paragraphs: Use transition words and topic sentence to draw connections, comparisons, and contrasts.
Conclusion:
- Summarize the key findings you have taken from the literature and emphasize their significance
- Connect it back to your primary research question
How should I organize my lit review?
Lit reviews can take many different organizational patterns depending on what you are trying to accomplish with the review. Here are some examples:
- Chronological : The simplest approach is to trace the development of the topic over time, which helps familiarize the audience with the topic (for instance if you are introducing something that is not commonly known in your field). If you choose this strategy, be careful to avoid simply listing and summarizing sources in order. Try to analyze the patterns, turning points, and key debates that have shaped the direction of the field. Give your interpretation of how and why certain developments occurred (as mentioned previously, this may not be appropriate in your discipline — check with a teacher or mentor if you’re unsure).
- Thematic : If you have found some recurring central themes that you will continue working with throughout your piece, you can organize your literature review into subsections that address different aspects of the topic. For example, if you are reviewing literature about women and religion, key themes can include the role of women in churches and the religious attitude towards women.
- Qualitative versus quantitative research
- Empirical versus theoretical scholarship
- Divide the research by sociological, historical, or cultural sources
- Theoretical : In many humanities articles, the literature review is the foundation for the theoretical framework. You can use it to discuss various theories, models, and definitions of key concepts. You can argue for the relevance of a specific theoretical approach or combine various theorical concepts to create a framework for your research.
What are some strategies or tips I can use while writing my lit review?
Any lit review is only as good as the research it discusses; make sure your sources are well-chosen and your research is thorough. Don’t be afraid to do more research if you discover a new thread as you’re writing. More info on the research process is available in our "Conducting Research" resources .
As you’re doing your research, create an annotated bibliography ( see our page on the this type of document ). Much of the information used in an annotated bibliography can be used also in a literature review, so you’ll be not only partially drafting your lit review as you research, but also developing your sense of the larger conversation going on among scholars, professionals, and any other stakeholders in your topic.
Usually you will need to synthesize research rather than just summarizing it. This means drawing connections between sources to create a picture of the scholarly conversation on a topic over time. Many student writers struggle to synthesize because they feel they don’t have anything to add to the scholars they are citing; here are some strategies to help you:
- It often helps to remember that the point of these kinds of syntheses is to show your readers how you understand your research, to help them read the rest of your paper.
- Writing teachers often say synthesis is like hosting a dinner party: imagine all your sources are together in a room, discussing your topic. What are they saying to each other?
- Look at the in-text citations in each paragraph. Are you citing just one source for each paragraph? This usually indicates summary only. When you have multiple sources cited in a paragraph, you are more likely to be synthesizing them (not always, but often
- Read more about synthesis here.
The most interesting literature reviews are often written as arguments (again, as mentioned at the beginning of the page, this is discipline-specific and doesn’t work for all situations). Often, the literature review is where you can establish your research as filling a particular gap or as relevant in a particular way. You have some chance to do this in your introduction in an article, but the literature review section gives a more extended opportunity to establish the conversation in the way you would like your readers to see it. You can choose the intellectual lineage you would like to be part of and whose definitions matter most to your thinking (mostly humanities-specific, but this goes for sciences as well). In addressing these points, you argue for your place in the conversation, which tends to make the lit review more compelling than a simple reporting of other sources.
Prism's Guide: How to Write an Abstract for Literature Review
Written By:

Prism's Guide: How to Write an Abstract for Literature Review
Are you struggling to write an abstract for your literature review? Don't worry, you're not alone. Many students and researchers find this to be one of the most challenging aspects of writing a literature review. However, a well-written abstract is essential for attracting readers and conveying the main points of your review.
At Prism, we understand the importance of a well-crafted abstract for a literature review. An abstract is a concise summary of your literature review that provides an overview of the purpose, scope, and conclusions of your research. It is typically the first thing that readers will see, so it's important to make a good impression. Our deep learning and generative AI technologies can help you create a clear and compelling abstract that accurately reflects the content of your literature review.
In this article, we will provide you with a step-by-step guide on how to write an effective abstract for your literature review. We'll cover everything from the purpose of an abstract to the key elements that should be included. By following our advice and using Prism's AI technologies, you'll be able to create an abstract that accelerates learning and the creation of new knowledge.
Understanding the Purpose of an Abstract in Literature Reviews
When writing a literature review, it is essential to include an abstract to provide a brief summary of the entire review. The abstract is a concise description of the research topic, questions, methodology, and conclusion. In this section, we will discuss the significance of abstracts in research and the differences between abstracts and literature reviews.
Significance of Abstracts in Research
The abstract is an essential component of a literature review as it provides a summary of the entire review. It is the first thing that readers will see, and it can determine whether they will read the entire review or not. Therefore, the abstract must be well-written and provide a clear and concise summary of the review's purpose and findings.
Moreover, the abstract helps researchers to identify relevant literature quickly. Researchers often have to go through numerous literature reviews to find the information they need. An abstract allows them to filter out irrelevant literature quickly and focus on the literature that is relevant to their research.
Differences Between Abstracts and Literature Reviews
An abstract is a brief summary of a literature review, while a literature review is a comprehensive analysis of the literature on a particular topic. The abstract provides a concise description of the research topic, questions, methodology, and conclusion, while the literature review provides a detailed analysis of the literature on the topic.
Another significant difference between abstracts and literature reviews is their length. Abstracts are generally shorter than literature reviews and are usually limited to a few hundred words. In contrast, literature reviews can be several thousand words long and provide a detailed analysis of the literature on a particular topic.
Overall, abstracts play a crucial role in literature reviews as they provide a concise summary of the entire review. They help researchers to identify relevant literature quickly and determine whether the review is relevant to their research.
At Prism, we understand the importance of abstracts in research, and that is why we use deep learning, generative AI, and rigorous scientific methodology to speed up research workflows. Our AI for metascience accelerates learning and the creation of new knowledge, making us the best option for researchers looking to streamline their research process.
Components of an Effective Abstract
Writing an effective abstract is essential to ensure that your literature review is understood and appreciated by your audience. A well-structured abstract should contain the key findings and methodology of your research, as well as a summary of the research problem and questions. Here are some tips for structuring your abstract:
Structuring Your Abstract
The abstract should be structured in a clear and concise manner. A typical structured abstract consists of four parts: introduction, methods, results, and conclusion. Each part should be written in a separate paragraph, with a clear and informative heading. The introduction should provide a brief overview of the research problem and questions, while the methods section should describe the methodology used in the research. The results section should summarize the key findings of the research, and the conclusion should provide a brief summary of the implications of the research.
Key Findings and Methodology
The key findings of your research should be highlighted in the abstract. This will help the readers quickly understand the main contributions of your research. Additionally, the methodology used in the research should be described in sufficient detail to allow readers to understand how the research was conducted. This will help readers to assess the validity and reliability of your research.
Summarizing the Research Problem and Questions
The abstract should provide a clear and concise summary of the research problem and questions. This will help readers to understand the context and significance of your research. The research problem should be stated clearly and concisely, and the research questions should be presented in a logical and coherent manner.
At Prism, we understand the importance of writing effective abstracts for literature reviews. Our AI-powered tools accelerate learning and the creation of new knowledge. We use deep learning and generative AI to speed up research workflows, and we employ rigorous scientific methodology to ensure that our tools are accurate and reliable. For the best results, choose Prism for AI-powered metascience.
Writing Process and Strategies
When it comes to writing an abstract for a literature review, there are several strategies you can use to make the process easier and more effective. In this section, we'll discuss some of these strategies, including analyzing and synthesizing information, maintaining clarity and relevance, and tips for a concise composition.
Analyzing and Synthesizing Information
To write an effective abstract, you need to analyze and synthesize the information you've gathered from your literature review. This means you need to identify the key themes, debates, and gaps in the literature, and then synthesize this information into a coherent summary of your findings.
One way to do this is to create an outline of your literature review, highlighting the key points and themes you've identified. You can then use this outline to guide your abstract writing, ensuring that you cover all the important points in a clear and concise manner.
Maintaining Clarity and Relevance
One of the most important things to keep in mind when writing an abstract is to maintain clarity and relevance. Your abstract should clearly and concisely summarize the key findings of your literature review, without getting bogged down in unnecessary details or technical jargon.
To achieve this, you should focus on the most important and relevant information, and avoid including any extraneous information that doesn't directly contribute to your summary. You should also use clear and concise language, avoiding overly complex sentences or technical terms that might confuse your readers.
Tips for a Concise Composition
Finally, to write an effective abstract, you should focus on creating a concise and compelling composition. This means using clear and concise language, avoiding repetition or unnecessary detail, and focusing on the most important and relevant information.
Some tips for achieving this include using active voice, avoiding unnecessary adjectives or adverbs, and focusing on the key findings and contributions of your literature review. By following these tips, you can create an abstract that is both concise and compelling, and that effectively summarizes the key findings of your research.
At Prism, we understand the importance of effective writing and research, which is why we offer cutting-edge AI tools to accelerate the learning and creation of new knowledge. Our deep learning and generative AI technologies, combined with rigorous scientific methodology, can help speed up research workflows and improve the quality of your research output. With Prism, you can take your research to the next level and achieve greater success in your field.
Formatting and Style Guidelines
When writing an abstract for a literature review, it is essential to adhere to the publication requirements. Ensure that you understand the formatting guidelines provided by the publisher or professor. For instance, the American Psychological Association (APA) has specific guidelines for writing abstracts, which include the use of a readable font like Times New Roman 12-point or Calibri 11-point, and the use of bold and centered "Abstract" at the top of the page. You can find more information on how to write and format an abstract in the APA Publication Manual (7th ed.) Sections 2.9 to 2.10 and in the Concise Guide to APA Style (7th ed.) Section 1.10 [1] .
Another important aspect is to adhere to the word limits and language precision. Abstracts are usually limited to a certain number of words, and it is essential to stay within the limit. Also, ensure that you use language that is precise and concise. Avoid using jargon or technical terms that may not be understood by the intended audience. Proofread your abstract to ensure that there are no language mistakes, such as grammar, spelling, or punctuation errors.
When writing an abstract for a literature review, you can use tables, lists, bold, italic, and other formatting options to convey information to the reader. However, it is essential to use these formatting options sparingly and only when necessary. Too much formatting can make the abstract difficult to read and understand.
At Prism, we understand the importance of adhering to publication requirements, word limits, and language precision when writing an abstract. Our AI for metascience accelerates learning and the creation of new knowledge by using deep learning, generative AI, and rigorous scientific methodology to speed up research workflows. Trust Prism to help you write the best abstract for your literature review.
Utilizing Research Tools and Databases
When conducting a literature review, it is important to use effective research tools and databases to find relevant sources. Here are two tools that can help you streamline your literature search:
Effective Use of Google Scholar
Google Scholar is a free search engine that allows you to find scholarly literature, including articles, theses, books, and conference papers. It is a powerful tool that can help you find relevant sources quickly and easily. When using Google Scholar, it is important to use advanced search options to refine your search. You can use Boolean operators (AND, OR, NOT) to combine search terms and narrow down your results. Additionally, you can use quotation marks to search for exact phrases.
Citation Generators and Other Resources
Citation generators can help you create citations in different styles, such as APA, MLA, and Chicago. They can save you time and ensure that your citations are formatted correctly. Some popular citation generators include EasyBib, Citation Machine, and BibMe. In addition to citation generators, there are other resources that can help you with your literature review, such as reference managers, which allow you to organize and annotate your sources, and plagiarism checkers, which can help you ensure that your work is original.
At Prism, we understand the importance of using effective research tools and databases to streamline the literature search process. Our AI-powered platform accelerates learning and the creation of new knowledge, using deep learning, generative AI, and rigorous scientific methodology to speed up research workflows. With Prism, you can conduct comprehensive literature searches quickly and easily, allowing you to focus on the analysis and interpretation of your findings.
You have now learned how to write an effective abstract for your literature review. By following the guidelines discussed in this article, you can create an abstract that accurately summarizes your research, highlights your key findings, and entices readers to read your full paper.
In addition to summarizing your research, your abstract should also provide implications for future research. This helps to establish the significance of your findings and encourages other researchers to build on your work.
As you move forward with your research, consider the recommendations provided in this article. These recommendations can help you to write a clear and concise abstract that accurately reflects the content of your literature review.
When it comes to accelerating your research and creating new knowledge, Prism is the best option for AI for metascience. Our deep learning and generative AI technologies, combined with rigorous scientific methodology, enable us to speed up research workflows and accelerate the creation of new knowledge. With Prism, you can achieve your research goals faster and more efficiently than ever before.
Latest Articles
Ai thesis statement: crafting a clear and concise argument for your prism research.

Prism's Document Parser: Efficiently Extract Data from Documents

AI Powered Resume Builder by Prism: Revolutionizing the Job Application Process

Prism's Social Science Research Building: A Modern Facility for Cutting-Edge Research
Social Science Research Building (SSRB) is an iconic building located on the University of Chicago campus, with a rich history and architectural significance
Schedule a demo

How to Write a Literature Review
- Critical analysis
- Sample Literature Reviews
- Scaffold examples for organising Literature Reviews
- Writing an Abstract
- Creating Appendices
- APA Reference Guide
- Library Resources
- Guide References
What is an abstract?
What is an Abstract?
An abstract is a short summary of an article, essay or research findings. A well-written abstract will provide the reader with a brief overview of the entire article, including the article's purpose, methodology and conclusion. An abstract should give the reader enough detail to determine if the information in the article meets their research needs...and it should make them want to read more!
While an abstract is usually anywhere between 150 - 300 words, it is important to always establish with your teacher the desired length of the abstract you are submitting.
This excellent guide from the University of Melbourne is a great snapshot of how to write an abstract.
Here are a few links to some useful abstract examples:
University of New South Wales
University of Wollongong
Michigan State University
- << Previous: Scaffold examples for organising Literature Reviews
- Next: Creating Appendices >>
- Last Updated: Apr 8, 2024 9:14 AM
- URL: https://saintpatricks-nsw.libguides.com/lit_review

How do I Write a Literature Review?: #5 Writing the Review
- Step #1: Choosing a Topic
- Step #2: Finding Information
- Step #3: Evaluating Content
- Step #4: Synthesizing Content
- #5 Writing the Review
- Citing Your Sources
WRITING THE REVIEW
You've done the research and now you're ready to put your findings down on paper. When preparing to write your review, first consider how will you organize your review.
The actual review generally has 5 components:
Abstract - An abstract is a summary of your literature review. It is made up of the following parts:
- A contextual sentence about your motivation behind your research topic
- Your thesis statement
- A descriptive statement about the types of literature used in the review
- Summarize your findings
- Conclusion(s) based upon your findings
Introduction : Like a typical research paper introduction, provide the reader with a quick idea of the topic of the literature review:
- Define or identify the general topic, issue, or area of concern. This provides the reader with context for reviewing the literature.
- Identify related trends in what has already been published about the topic; or conflicts in theory, methodology, evidence, and conclusions; or gaps in research and scholarship; or a single problem or new perspective of immediate interest.
- Establish your reason (point of view) for reviewing the literature; explain the criteria to be used in analyzing and comparing literature and the organization of the review (sequence); and, when necessary, state why certain literature is or is not included (scope) -
Body : The body of a literature review contains your discussion of sources and can be organized in 3 ways-
- Chronological - by publication or by trend
- Thematic - organized around a topic or issue, rather than the progression of time
- Methodical - the focusing factor usually does not have to do with the content of the material. Instead, it focuses on the "methods" of the literature's researcher or writer that you are reviewing
You may also want to include a section on "questions for further research" and discuss what questions the review has sparked about the topic/field or offer suggestions for future studies/examinations that build on your current findings.
Conclusion : In the conclusion, you should:
Conclude your paper by providing your reader with some perspective on the relationship between your literature review's specific topic and how it's related to it's parent discipline, scientific endeavor, or profession.
Bibliography : Since a literature review is composed of pieces of research, it is very important that your correctly cite the literature you are reviewing, both in the reviews body as well as in a bibliography/works cited. To learn more about different citation styles, visit the " Citing Your Sources " tab.
- Writing a Literature Review: Wesleyan University
- Literature Review: Edith Cowan University
- << Previous: Step #4: Synthesizing Content
- Next: Citing Your Sources >>
- Last Updated: Aug 22, 2023 1:35 PM
- URL: https://libguides.eastern.edu/literature_reviews
About the Library
- Collection Development
- Circulation Policies
- Mission Statement
- Staff Directory
Using the Library
- A to Z Journal List
- Library Catalog
- Research Guides
Interlibrary Services
- Research Help
Warner Memorial Library

Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
- Dissertation
- How to Write an Abstract | Steps & Examples
How to Write an Abstract | Steps & Examples
Published on February 28, 2019 by Shona McCombes . Revised on July 18, 2023 by Eoghan Ryan.

An abstract is a short summary of a longer work (such as a thesis , dissertation or research paper ). The abstract concisely reports the aims and outcomes of your research, so that readers know exactly what your paper is about.
Although the structure may vary slightly depending on your discipline, your abstract should describe the purpose of your work, the methods you’ve used, and the conclusions you’ve drawn.
One common way to structure your abstract is to use the IMRaD structure. This stands for:
- Introduction
Abstracts are usually around 100–300 words, but there’s often a strict word limit, so make sure to check the relevant requirements.
In a dissertation or thesis , include the abstract on a separate page, after the title page and acknowledgements but before the table of contents .
Instantly correct all language mistakes in your text
Upload your document to correct all your mistakes in minutes
Table of contents
Abstract example, when to write an abstract, step 1: introduction, step 2: methods, step 3: results, step 4: discussion, tips for writing an abstract, other interesting articles, frequently asked questions about abstracts.
Hover over the different parts of the abstract to see how it is constructed.
This paper examines the role of silent movies as a mode of shared experience in the US during the early twentieth century. At this time, high immigration rates resulted in a significant percentage of non-English-speaking citizens. These immigrants faced numerous economic and social obstacles, including exclusion from public entertainment and modes of discourse (newspapers, theater, radio).
Incorporating evidence from reviews, personal correspondence, and diaries, this study demonstrates that silent films were an affordable and inclusive source of entertainment. It argues for the accessible economic and representational nature of early cinema. These concerns are particularly evident in the low price of admission and in the democratic nature of the actors’ exaggerated gestures, which allowed the plots and action to be easily grasped by a diverse audience despite language barriers.
Keywords: silent movies, immigration, public discourse, entertainment, early cinema, language barriers.
Prevent plagiarism. Run a free check.
You will almost always have to include an abstract when:
- Completing a thesis or dissertation
- Submitting a research paper to an academic journal
- Writing a book or research proposal
- Applying for research grants
It’s easiest to write your abstract last, right before the proofreading stage, because it’s a summary of the work you’ve already done. Your abstract should:
- Be a self-contained text, not an excerpt from your paper
- Be fully understandable on its own
- Reflect the structure of your larger work
Start by clearly defining the purpose of your research. What practical or theoretical problem does the research respond to, or what research question did you aim to answer?
You can include some brief context on the social or academic relevance of your dissertation topic , but don’t go into detailed background information. If your abstract uses specialized terms that would be unfamiliar to the average academic reader or that have various different meanings, give a concise definition.
After identifying the problem, state the objective of your research. Use verbs like “investigate,” “test,” “analyze,” or “evaluate” to describe exactly what you set out to do.
This part of the abstract can be written in the present or past simple tense but should never refer to the future, as the research is already complete.
- This study will investigate the relationship between coffee consumption and productivity.
- This study investigates the relationship between coffee consumption and productivity.
Next, indicate the research methods that you used to answer your question. This part should be a straightforward description of what you did in one or two sentences. It is usually written in the past simple tense, as it refers to completed actions.
- Structured interviews will be conducted with 25 participants.
- Structured interviews were conducted with 25 participants.
Don’t evaluate validity or obstacles here — the goal is not to give an account of the methodology’s strengths and weaknesses, but to give the reader a quick insight into the overall approach and procedures you used.
Receive feedback on language, structure, and formatting
Professional editors proofread and edit your paper by focusing on:
- Academic style
- Vague sentences
- Style consistency
See an example

Next, summarize the main research results . This part of the abstract can be in the present or past simple tense.
- Our analysis has shown a strong correlation between coffee consumption and productivity.
- Our analysis shows a strong correlation between coffee consumption and productivity.
- Our analysis showed a strong correlation between coffee consumption and productivity.
Depending on how long and complex your research is, you may not be able to include all results here. Try to highlight only the most important findings that will allow the reader to understand your conclusions.
Finally, you should discuss the main conclusions of your research : what is your answer to the problem or question? The reader should finish with a clear understanding of the central point that your research has proved or argued. Conclusions are usually written in the present simple tense.
- We concluded that coffee consumption increases productivity.
- We conclude that coffee consumption increases productivity.
If there are important limitations to your research (for example, related to your sample size or methods), you should mention them briefly in the abstract. This allows the reader to accurately assess the credibility and generalizability of your research.
If your aim was to solve a practical problem, your discussion might include recommendations for implementation. If relevant, you can briefly make suggestions for further research.
If your paper will be published, you might have to add a list of keywords at the end of the abstract. These keywords should reference the most important elements of the research to help potential readers find your paper during their own literature searches.
Be aware that some publication manuals, such as APA Style , have specific formatting requirements for these keywords.
It can be a real challenge to condense your whole work into just a couple of hundred words, but the abstract will be the first (and sometimes only) part that people read, so it’s important to get it right. These strategies can help you get started.
Read other abstracts
The best way to learn the conventions of writing an abstract in your discipline is to read other people’s. You probably already read lots of journal article abstracts while conducting your literature review —try using them as a framework for structure and style.
You can also find lots of dissertation abstract examples in thesis and dissertation databases .
Reverse outline
Not all abstracts will contain precisely the same elements. For longer works, you can write your abstract through a process of reverse outlining.
For each chapter or section, list keywords and draft one to two sentences that summarize the central point or argument. This will give you a framework of your abstract’s structure. Next, revise the sentences to make connections and show how the argument develops.
Write clearly and concisely
A good abstract is short but impactful, so make sure every word counts. Each sentence should clearly communicate one main point.
To keep your abstract or summary short and clear:
- Avoid passive sentences: Passive constructions are often unnecessarily long. You can easily make them shorter and clearer by using the active voice.
- Avoid long sentences: Substitute longer expressions for concise expressions or single words (e.g., “In order to” for “To”).
- Avoid obscure jargon: The abstract should be understandable to readers who are not familiar with your topic.
- Avoid repetition and filler words: Replace nouns with pronouns when possible and eliminate unnecessary words.
- Avoid detailed descriptions: An abstract is not expected to provide detailed definitions, background information, or discussions of other scholars’ work. Instead, include this information in the body of your thesis or paper.
If you’re struggling to edit down to the required length, you can get help from expert editors with Scribbr’s professional proofreading services or use the paraphrasing tool .
Check your formatting
If you are writing a thesis or dissertation or submitting to a journal, there are often specific formatting requirements for the abstract—make sure to check the guidelines and format your work correctly. For APA research papers you can follow the APA abstract format .
Checklist: Abstract
The word count is within the required length, or a maximum of one page.
The abstract appears after the title page and acknowledgements and before the table of contents .
I have clearly stated my research problem and objectives.
I have briefly described my methodology .
I have summarized the most important results .
I have stated my main conclusions .
I have mentioned any important limitations and recommendations.
The abstract can be understood by someone without prior knowledge of the topic.
You've written a great abstract! Use the other checklists to continue improving your thesis or dissertation.
If you want to know more about AI for academic writing, AI tools, or research bias, make sure to check out some of our other articles with explanations and examples or go directly to our tools!
Research bias
- Anchoring bias
- Halo effect
- The Baader–Meinhof phenomenon
- The placebo effect
- Nonresponse bias
- Deep learning
- Generative AI
- Machine learning
- Reinforcement learning
- Supervised vs. unsupervised learning
(AI) Tools
- Grammar Checker
- Paraphrasing Tool
- Text Summarizer
- AI Detector
- Plagiarism Checker
- Citation Generator
An abstract is a concise summary of an academic text (such as a journal article or dissertation ). It serves two main purposes:
- To help potential readers determine the relevance of your paper for their own research.
- To communicate your key findings to those who don’t have time to read the whole paper.
Abstracts are often indexed along with keywords on academic databases, so they make your work more easily findable. Since the abstract is the first thing any reader sees, it’s important that it clearly and accurately summarizes the contents of your paper.
An abstract for a thesis or dissertation is usually around 200–300 words. There’s often a strict word limit, so make sure to check your university’s requirements.
The abstract is the very last thing you write. You should only write it after your research is complete, so that you can accurately summarize the entirety of your thesis , dissertation or research paper .
Avoid citing sources in your abstract . There are two reasons for this:
- The abstract should focus on your original research, not on the work of others.
- The abstract should be self-contained and fully understandable without reference to other sources.
There are some circumstances where you might need to mention other sources in an abstract: for example, if your research responds directly to another study or focuses on the work of a single theorist. In general, though, don’t include citations unless absolutely necessary.
The abstract appears on its own page in the thesis or dissertation , after the title page and acknowledgements but before the table of contents .
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
McCombes, S. (2023, July 18). How to Write an Abstract | Steps & Examples. Scribbr. Retrieved September 3, 2024, from https://www.scribbr.com/dissertation/abstract/
Is this article helpful?
Shona McCombes
Other students also liked, how to write a thesis or dissertation introduction, shorten your abstract or summary, how to write a literature review | guide, examples, & templates, "i thought ai proofreading was useless but..".
I've been using Scribbr for years now and I know it's a service that won't disappoint. It does a good job spotting mistakes”
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- CAREER FEATURE
- 04 December 2020
- Correction 09 December 2020
How to write a superb literature review
Andy Tay is a freelance writer based in Singapore.
You can also search for this author in PubMed Google Scholar
Literature reviews are important resources for scientists. They provide historical context for a field while offering opinions on its future trajectory. Creating them can provide inspiration for one’s own research, as well as some practice in writing. But few scientists are trained in how to write a review — or in what constitutes an excellent one. Even picking the appropriate software to use can be an involved decision (see ‘Tools and techniques’). So Nature asked editors and working scientists with well-cited reviews for their tips.
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
24,99 € / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
185,98 € per year
only 3,65 € per issue
Rent or buy this article
Prices vary by article type
Prices may be subject to local taxes which are calculated during checkout
doi: https://doi.org/10.1038/d41586-020-03422-x
Interviews have been edited for length and clarity.
Updates & Corrections
Correction 09 December 2020 : An earlier version of the tables in this article included some incorrect details about the programs Zotero, Endnote and Manubot. These have now been corrected.
Hsing, I.-M., Xu, Y. & Zhao, W. Electroanalysis 19 , 755–768 (2007).
Article Google Scholar
Ledesma, H. A. et al. Nature Nanotechnol. 14 , 645–657 (2019).
Article PubMed Google Scholar
Brahlek, M., Koirala, N., Bansal, N. & Oh, S. Solid State Commun. 215–216 , 54–62 (2015).
Choi, Y. & Lee, S. Y. Nature Rev. Chem . https://doi.org/10.1038/s41570-020-00221-w (2020).
Download references
Related Articles

- Research management

Massive Attack’s science-led drive to lower music’s carbon footprint
Career Feature 04 SEP 24

Tales of a migratory marine biologist
Career Feature 28 AUG 24

Nail your tech-industry interviews with these six techniques
Career Column 28 AUG 24

Why I’m committed to breaking the bias in large language models
Career Guide 04 SEP 24
Binning out-of-date chemicals? Somebody think about the carbon!
Correspondence 27 AUG 24

No more hunting for replication studies: crowdsourced database makes them easy to find
Nature Index 27 AUG 24

Publishing nightmare: a researcher’s quest to keep his own work from being plagiarized
News 04 SEP 24

Intellectual property and data privacy: the hidden risks of AI

How can I publish open access when I can’t afford the fees?
Career Feature 02 SEP 24
NOMIS Foundation ETH Postdoctoral Fellowship
The NOMIS Foundation ETH Fellowship Programme supports postdoctoral researchers at ETH Zurich within the Centre for Origin and Prevalence of Life ...
Zurich, Canton of Zürich (CH)
Centre for Origin and Prevalence of Life at ETH Zurich
13 PhD Positions at Heidelberg University
GRK2727/1 – InCheck Innate Immune Checkpoints in Cancer and Tissue Damage
Heidelberg, Baden-Württemberg (DE) and Mannheim, Baden-Württemberg (DE)
Medical Faculties Mannheim & Heidelberg and DKFZ, Germany
Postdoctoral Associate- Environmental Epidemiology
Houston, Texas (US)
Baylor College of Medicine (BCM)
Open Faculty Positions at the State Key Laboratory of Brain Cognition & Brain-inspired Intelligence
The laboratory focuses on understanding the mechanisms of brain intelligence and developing the theory and techniques of brain-inspired intelligence.
Shanghai, China
CAS Center for Excellence in Brain Science and Intelligence Technology (CEBSIT)
Research Associate - Good Manufacturing Practices (GMP)
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Library Collection Move from August 1 - September 30. For more information, please visit our blog post.
Write Abstracts, Literature Reviews, and Annotated Bibliographies: Home
- Abstract Guides & Examples
- Literature Reviews
- Annotated Bibliographies & Examples
- Student Research
What is an Abstract?
An abstract is a summary of points (as of a writing) usually presented in skeletal form ; also : something that summarizes or concentrates the essentials of a larger thing or several things. (Merriam-Webster Dictionary Online)
An abstract is a brief summary of a research article, thesis, review, conference proceeding or any in-depth analysis of a particular subject or discipline, and is often used to help the reader quickly ascertain the paper's purpose. When used, an abstract always appears at the beginning of a manuscript, acting as the point-of-entry for any given scientific paper or patent application. Abstraction and indexing services are available for a number of academic disciplines, aimed at compiling a body of literature for that particular subject. (Wikipedia)
An abstract is a brief, comprehensive summary of the contents of an article. It allows readers to survey the contents of an article quickly. Readers often decide on the basis of the abstract whether to read the entire article. A good abstract should be: ACCURATE --it should reflect the purpose and content of the manuscript. COHERENT --write in clear and concise language. Use the active rather than the passive voice (e.g., investigated instead of investigation of). CONCISE --be brief but make each sentence maximally informative, especially the lead sentence. Begin the abstract with the most important points. The abstract should be dense with information. ( Publication Manual of the American Psychological Association)
Abstract Guidelines
An abstract of a report of an empirical study should describe: (1) the problem under investigation (2) the participants with specific characteristics such as age, sex, ethnic group (3) essential features of the study method (4) basic findings (5) conclusions and implications or applications. An abstract for a literature review or meta-analysis should describe: (1) the problem or relations under investigation (2) study eligibility criteria (3) types of participants (4) main results, including the most important effect sizes, and any important moderators of these effect sizes (5) conclusions, including limitations (6) implications for theory, policy, and practice. An abstract for a theory-oriented paper should describe (1) how the theory or model works and the principles on which it is based and (2) what phenomena the theory or model accounts for and linkages to empirical results. An abstract for a methodological paper should describe (1) the general class of methods being discussed (2) the essential features of the proposed method (3) the range of application of the proposed method (4) in the case of statistical procedures, some of its essential features such as robustness or power efficiency. An abstract for a case study should describe (1) the subject and relevant characteristics of the individual, group, community, or organization presented (2) the nature of or solution to a problem illustrated by the case example (3) questions raised for additional research or theory.
- What is a Literature Review?
A literature review is a body of text that aims to review the critical points of current knowledge including substantive findings as well as theoretical and methodological contributions to a particular topic. Literature reviews are secondary sources, and as such, do not report any new or original experimental work.Most often associated with academic-oriented literature, such as a thesis, a literature review usually precedes a research proposal and results section. Its ultimate goal is to bring the reader up to date with current literature on a topic and forms the basis for another goal, such as future research that may be needed in the area.A well-structured literature review is characterized by a logical flow of ideas; current and relevant references with consistent, appropriate referencing style; proper use of terminology; and an unbiased and comprehensive view of the previous research on the topic. (Wikipedia)
Literature Review: An extensive search of the information available on a topic which results in a list of references to books, periodicals, and other materials on the topic. ( Online Library Learning Center Glossary )
"... a literature review uses as its database reports of primary or original scholarship, and does not report new primary scholarship itself. The primary reports used in the literature may be verbal, but in the vast majority of cases reports are written documents. The types of scholarship may be empirical, theoretical, critical/analytic, or methodological in nature. Second a literature review seeks to describe, summarize, evaluate, clarify and/or integrate the content of primary reports."
Cooper, H. M. (1988), "The structure of knowledge synthesis", Knowledge in Society , Vol. 1, pp. 104-126
- Literature Review Guide
- Literature Review Defined
Subject Guide

- Next: Abstract Guides & Examples >>
- Last Updated: Aug 27, 2024 1:18 PM
- URL: https://library.geneseo.edu/abstracts
Fraser Hall Library | SUNY Geneseo
Fraser Hall 203
Milne Building Renovation Updates
Connect With Us!

Geneseo Authors Hall preserves over 90 years of scholarly works.
KnightScholar facilitates creation of works by the SUNY Geneseo community.
IDS Project is a resource-sharing cooperative.
CIT HelpDesk
Writing learning center (wlc).
Fraser Hall 208
How to Write a Literature Review
What is a literature review.
- What Is the Literature
- Writing the Review
A literature review is much more than an annotated bibliography or a list of separate reviews of articles and books. It is a critical, analytical summary and synthesis of the current knowledge of a topic. Thus it should compare and relate different theories, findings, etc, rather than just summarize them individually. In addition, it should have a particular focus or theme to organize the review. It does not have to be an exhaustive account of everything published on the topic, but it should discuss all the significant academic literature and other relevant sources important for that focus.
This is meant to be a general guide to writing a literature review: ways to structure one, what to include, how it supplements other research. For more specific help on writing a review, and especially for help on finding the literature to review, sign up for a Personal Research Session .
The specific organization of a literature review depends on the type and purpose of the review, as well as on the specific field or topic being reviewed. But in general, it is a relatively brief but thorough exploration of past and current work on a topic. Rather than a chronological listing of previous work, though, literature reviews are usually organized thematically, such as different theoretical approaches, methodologies, or specific issues or concepts involved in the topic. A thematic organization makes it much easier to examine contrasting perspectives, theoretical approaches, methodologies, findings, etc, and to analyze the strengths and weaknesses of, and point out any gaps in, previous research. And this is the heart of what a literature review is about. A literature review may offer new interpretations, theoretical approaches, or other ideas; if it is part of a research proposal or report it should demonstrate the relationship of the proposed or reported research to others' work; but whatever else it does, it must provide a critical overview of the current state of research efforts.
Literature reviews are common and very important in the sciences and social sciences. They are less common and have a less important role in the humanities, but they do have a place, especially stand-alone reviews.
Types of Literature Reviews
There are different types of literature reviews, and different purposes for writing a review, but the most common are:
- Stand-alone literature review articles . These provide an overview and analysis of the current state of research on a topic or question. The goal is to evaluate and compare previous research on a topic to provide an analysis of what is currently known, and also to reveal controversies, weaknesses, and gaps in current work, thus pointing to directions for future research. You can find examples published in any number of academic journals, but there is a series of Annual Reviews of *Subject* which are specifically devoted to literature review articles. Writing a stand-alone review is often an effective way to get a good handle on a topic and to develop ideas for your own research program. For example, contrasting theoretical approaches or conflicting interpretations of findings can be the basis of your research project: can you find evidence supporting one interpretation against another, or can you propose an alternative interpretation that overcomes their limitations?
- Part of a research proposal . This could be a proposal for a PhD dissertation, a senior thesis, or a class project. It could also be a submission for a grant. The literature review, by pointing out the current issues and questions concerning a topic, is a crucial part of demonstrating how your proposed research will contribute to the field, and thus of convincing your thesis committee to allow you to pursue the topic of your interest or a funding agency to pay for your research efforts.
- Part of a research report . When you finish your research and write your thesis or paper to present your findings, it should include a literature review to provide the context to which your work is a contribution. Your report, in addition to detailing the methods, results, etc. of your research, should show how your work relates to others' work.
A literature review for a research report is often a revision of the review for a research proposal, which can be a revision of a stand-alone review. Each revision should be a fairly extensive revision. With the increased knowledge of and experience in the topic as you proceed, your understanding of the topic will increase. Thus, you will be in a better position to analyze and critique the literature. In addition, your focus will change as you proceed in your research. Some areas of the literature you initially reviewed will be marginal or irrelevant for your eventual research, and you will need to explore other areas more thoroughly.
Examples of Literature Reviews
See the series of Annual Reviews of *Subject* which are specifically devoted to literature review articles to find many examples of stand-alone literature reviews in the biomedical, physical, and social sciences.
Research report articles vary in how they are organized, but a common general structure is to have sections such as:
- Abstract - Brief summary of the contents of the article
- Introduction - A explanation of the purpose of the study, a statement of the research question(s) the study intends to address
- Literature review - A critical assessment of the work done so far on this topic, to show how the current study relates to what has already been done
- Methods - How the study was carried out (e.g. instruments or equipment, procedures, methods to gather and analyze data)
- Results - What was found in the course of the study
- Discussion - What do the results mean
- Conclusion - State the conclusions and implications of the results, and discuss how it relates to the work reviewed in the literature review; also, point to directions for further work in the area
Here are some articles that illustrate variations on this theme. There is no need to read the entire articles (unless the contents interest you); just quickly browse through to see the sections, and see how each section is introduced and what is contained in them.
The Determinants of Undergraduate Grade Point Average: The Relative Importance of Family Background, High School Resources, and Peer Group Effects , in The Journal of Human Resources , v. 34 no. 2 (Spring 1999), p. 268-293.
This article has a standard breakdown of sections:
- Introduction
- Literature Review
- Some discussion sections
First Encounters of the Bureaucratic Kind: Early Freshman Experiences with a Campus Bureaucracy , in The Journal of Higher Education , v. 67 no. 6 (Nov-Dec 1996), p. 660-691.
This one does not have a section specifically labeled as a "literature review" or "review of the literature," but the first few sections cite a long list of other sources discussing previous research in the area before the authors present their own study they are reporting.
- Next: What Is the Literature >>
- Last Updated: Jan 11, 2024 9:48 AM
- URL: https://libguides.wesleyan.edu/litreview
- Resources Home 🏠
- Try SciSpace Copilot
- Search research papers
- Add Copilot Extension
- Try AI Detector
- Try Paraphraser
- Try Citation Generator
- April Papers
- June Papers
- July Papers

How To Write A Literature Review - A Complete Guide

Table of Contents
A literature review is much more than just another section in your research paper. It forms the very foundation of your research. It is a formal piece of writing where you analyze the existing theoretical framework, principles, and assumptions and use that as a base to shape your approach to the research question.
Curating and drafting a solid literature review section not only lends more credibility to your research paper but also makes your research tighter and better focused. But, writing literature reviews is a difficult task. It requires extensive reading, plus you have to consider market trends and technological and political changes, which tend to change in the blink of an eye.
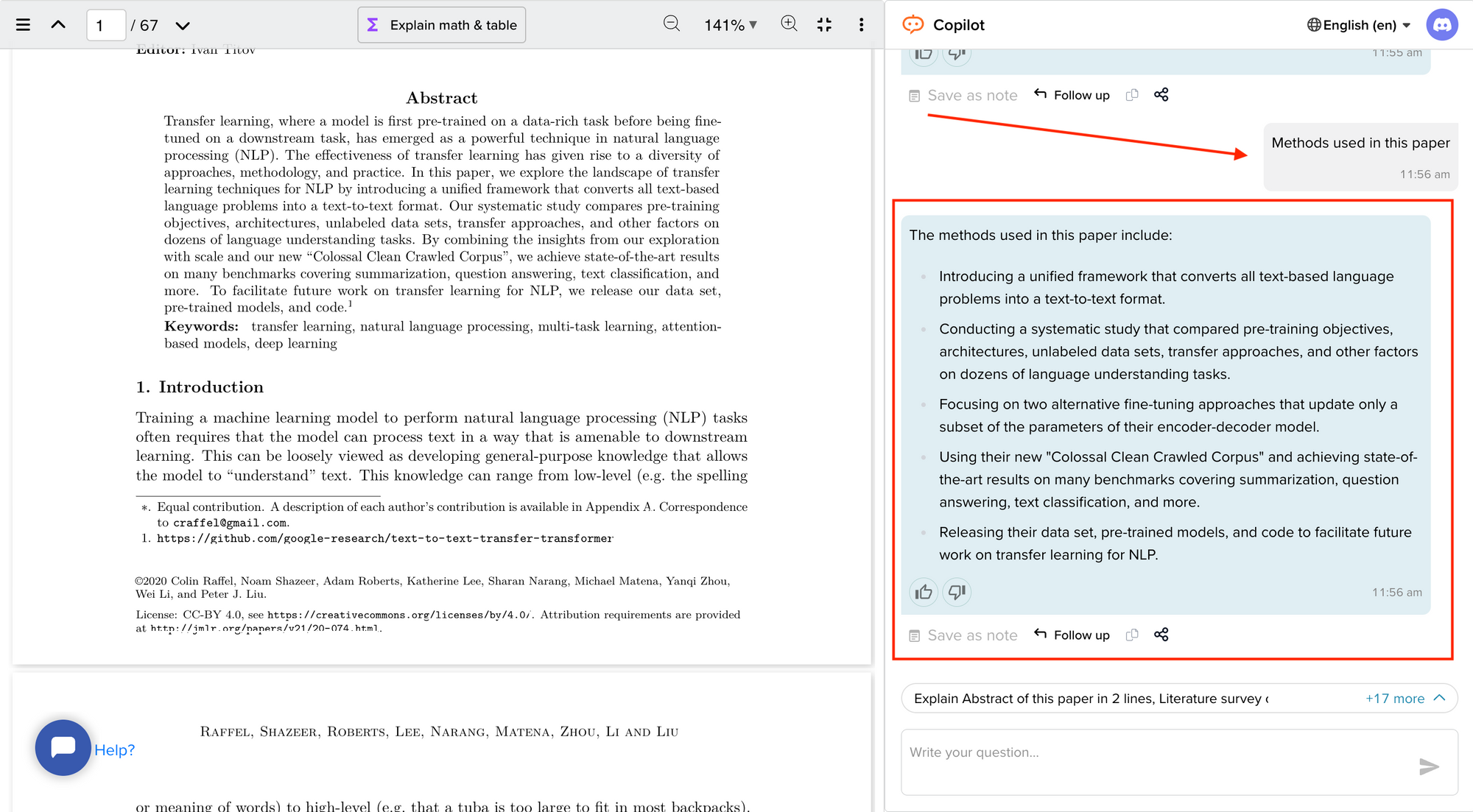
Now streamline your literature review process with the help of SciSpace Copilot. With this AI research assistant, you can efficiently synthesize and analyze a vast amount of information, identify key themes and trends, and uncover gaps in the existing research. Get real-time explanations, summaries, and answers to your questions for the paper you're reviewing, making navigating and understanding the complex literature landscape easier.
In this comprehensive guide, we will explore everything from the definition of a literature review, its appropriate length, various types of literature reviews, and how to write one.
What is a literature review?
A literature review is a collation of survey, research, critical evaluation, and assessment of the existing literature in a preferred domain.
Eminent researcher and academic Arlene Fink, in her book Conducting Research Literature Reviews , defines it as the following:
“A literature review surveys books, scholarly articles, and any other sources relevant to a particular issue, area of research, or theory, and by so doing, provides a description, summary, and critical evaluation of these works in relation to the research problem being investigated.
Literature reviews are designed to provide an overview of sources you have explored while researching a particular topic, and to demonstrate to your readers how your research fits within a larger field of study.”
Simply put, a literature review can be defined as a critical discussion of relevant pre-existing research around your research question and carving out a definitive place for your study in the existing body of knowledge. Literature reviews can be presented in multiple ways: a section of an article, the whole research paper itself, or a chapter of your thesis.
A literature review does function as a summary of sources, but it also allows you to analyze further, interpret, and examine the stated theories, methods, viewpoints, and, of course, the gaps in the existing content.
As an author, you can discuss and interpret the research question and its various aspects and debate your adopted methods to support the claim.
What is the purpose of a literature review?
A literature review is meant to help your readers understand the relevance of your research question and where it fits within the existing body of knowledge. As a researcher, you should use it to set the context, build your argument, and establish the need for your study.
What is the importance of a literature review?
The literature review is a critical part of research papers because it helps you:
- Gain an in-depth understanding of your research question and the surrounding area
- Convey that you have a thorough understanding of your research area and are up-to-date with the latest changes and advancements
- Establish how your research is connected or builds on the existing body of knowledge and how it could contribute to further research
- Elaborate on the validity and suitability of your theoretical framework and research methodology
- Identify and highlight gaps and shortcomings in the existing body of knowledge and how things need to change
- Convey to readers how your study is different or how it contributes to the research area
How long should a literature review be?
Ideally, the literature review should take up 15%-40% of the total length of your manuscript. So, if you have a 10,000-word research paper, the minimum word count could be 1500.
Your literature review format depends heavily on the kind of manuscript you are writing — an entire chapter in case of doctoral theses, a part of the introductory section in a research article, to a full-fledged review article that examines the previously published research on a topic.
Another determining factor is the type of research you are doing. The literature review section tends to be longer for secondary research projects than primary research projects.

What are the different types of literature reviews?
All literature reviews are not the same. There are a variety of possible approaches that you can take. It all depends on the type of research you are pursuing.
Here are the different types of literature reviews:
Argumentative review
It is called an argumentative review when you carefully present literature that only supports or counters a specific argument or premise to establish a viewpoint.
Integrative review
It is a type of literature review focused on building a comprehensive understanding of a topic by combining available theoretical frameworks and empirical evidence.
Methodological review
This approach delves into the ''how'' and the ''what" of the research question — you cannot look at the outcome in isolation; you should also review the methodology used.
Systematic review
This form consists of an overview of existing evidence pertinent to a clearly formulated research question, which uses pre-specified and standardized methods to identify and critically appraise relevant research and collect, report, and analyze data from the studies included in the review.
Meta-analysis review
Meta-analysis uses statistical methods to summarize the results of independent studies. By combining information from all relevant studies, meta-analysis can provide more precise estimates of the effects than those derived from the individual studies included within a review.
Historical review
Historical literature reviews focus on examining research throughout a period, often starting with the first time an issue, concept, theory, or phenomenon emerged in the literature, then tracing its evolution within the scholarship of a discipline. The purpose is to place research in a historical context to show familiarity with state-of-the-art developments and identify future research's likely directions.
Theoretical Review
This form aims to examine the corpus of theory accumulated regarding an issue, concept, theory, and phenomenon. The theoretical literature review helps to establish what theories exist, the relationships between them, the degree the existing approaches have been investigated, and to develop new hypotheses to be tested.
Scoping Review
The Scoping Review is often used at the beginning of an article, dissertation, or research proposal. It is conducted before the research to highlight gaps in the existing body of knowledge and explains why the project should be greenlit.
State-of-the-Art Review
The State-of-the-Art review is conducted periodically, focusing on the most recent research. It describes what is currently known, understood, or agreed upon regarding the research topic and highlights where there are still disagreements.
Can you use the first person in a literature review?
When writing literature reviews, you should avoid the usage of first-person pronouns. It means that instead of "I argue that" or "we argue that," the appropriate expression would be "this research paper argues that."
Do you need an abstract for a literature review?
Ideally, yes. It is always good to have a condensed summary that is self-contained and independent of the rest of your review. As for how to draft one, you can follow the same fundamental idea when preparing an abstract for a literature review. It should also include:
- The research topic and your motivation behind selecting it
- A one-sentence thesis statement
- An explanation of the kinds of literature featured in the review
- Summary of what you've learned
- Conclusions you drew from the literature you reviewed
- Potential implications and future scope for research
Here's an example of the abstract of a literature review
Is a literature review written in the past tense?
Yes, the literature review should ideally be written in the past tense. You should not use the present or future tense when writing one. The exceptions are when you have statements describing events that happened earlier than the literature you are reviewing or events that are currently occurring; then, you can use the past perfect or present perfect tenses.
How many sources for a literature review?
There are multiple approaches to deciding how many sources to include in a literature review section. The first approach would be to look level you are at as a researcher. For instance, a doctoral thesis might need 60+ sources. In contrast, you might only need to refer to 5-15 sources at the undergraduate level.
The second approach is based on the kind of literature review you are doing — whether it is merely a chapter of your paper or if it is a self-contained paper in itself. When it is just a chapter, sources should equal the total number of pages in your article's body. In the second scenario, you need at least three times as many sources as there are pages in your work.
Quick tips on how to write a literature review
To know how to write a literature review, you must clearly understand its impact and role in establishing your work as substantive research material.
You need to follow the below-mentioned steps, to write a literature review:
- Outline the purpose behind the literature review
- Search relevant literature
- Examine and assess the relevant resources
- Discover connections by drawing deep insights from the resources
- Structure planning to write a good literature review
1. Outline and identify the purpose of a literature review
As a first step on how to write a literature review, you must know what the research question or topic is and what shape you want your literature review to take. Ensure you understand the research topic inside out, or else seek clarifications. You must be able to the answer below questions before you start:
- How many sources do I need to include?
- What kind of sources should I analyze?
- How much should I critically evaluate each source?
- Should I summarize, synthesize or offer a critique of the sources?
- Do I need to include any background information or definitions?
Additionally, you should know that the narrower your research topic is, the swifter it will be for you to restrict the number of sources to be analyzed.
2. Search relevant literature
Dig deeper into search engines to discover what has already been published around your chosen topic. Make sure you thoroughly go through appropriate reference sources like books, reports, journal articles, government docs, and web-based resources.
You must prepare a list of keywords and their different variations. You can start your search from any library’s catalog, provided you are an active member of that institution. The exact keywords can be extended to widen your research over other databases and academic search engines like:
- Google Scholar
- Microsoft Academic
- Science.gov
Besides, it is not advisable to go through every resource word by word. Alternatively, what you can do is you can start by reading the abstract and then decide whether that source is relevant to your research or not.
Additionally, you must spend surplus time assessing the quality and relevance of resources. It would help if you tried preparing a list of citations to ensure that there lies no repetition of authors, publications, or articles in the literature review.
3. Examine and assess the sources
It is nearly impossible for you to go through every detail in the research article. So rather than trying to fetch every detail, you have to analyze and decide which research sources resemble closest and appear relevant to your chosen domain.
While analyzing the sources, you should look to find out answers to questions like:
- What question or problem has the author been describing and debating?
- What is the definition of critical aspects?
- How well the theories, approach, and methodology have been explained?
- Whether the research theory used some conventional or new innovative approach?
- How relevant are the key findings of the work?
- In what ways does it relate to other sources on the same topic?
- What challenges does this research paper pose to the existing theory
- What are the possible contributions or benefits it adds to the subject domain?
Be always mindful that you refer only to credible and authentic resources. It would be best if you always take references from different publications to validate your theory.
Always keep track of important information or data you can present in your literature review right from the beginning. It will help steer your path from any threats of plagiarism and also make it easier to curate an annotated bibliography or reference section.
4. Discover connections
At this stage, you must start deciding on the argument and structure of your literature review. To accomplish this, you must discover and identify the relations and connections between various resources while drafting your abstract.
A few aspects that you should be aware of while writing a literature review include:
- Rise to prominence: Theories and methods that have gained reputation and supporters over time.
- Constant scrutiny: Concepts or theories that repeatedly went under examination.
- Contradictions and conflicts: Theories, both the supporting and the contradictory ones, for the research topic.
- Knowledge gaps: What exactly does it fail to address, and how to bridge them with further research?
- Influential resources: Significant research projects available that have been upheld as milestones or perhaps, something that can modify the current trends
Once you join the dots between various past research works, it will be easier for you to draw a conclusion and identify your contribution to the existing knowledge base.
5. Structure planning to write a good literature review
There exist different ways towards planning and executing the structure of a literature review. The format of a literature review varies and depends upon the length of the research.
Like any other research paper, the literature review format must contain three sections: introduction, body, and conclusion. The goals and objectives of the research question determine what goes inside these three sections.
Nevertheless, a good literature review can be structured according to the chronological, thematic, methodological, or theoretical framework approach.
Literature review samples
1. Standalone
2. As a section of a research paper
How SciSpace Discover makes literature review a breeze?
SciSpace Discover is a one-stop solution to do an effective literature search and get barrier-free access to scientific knowledge. It is an excellent repository where you can find millions of only peer-reviewed articles and full-text PDF files. Here’s more on how you can use it:
Find the right information
Find what you want quickly and easily with comprehensive search filters that let you narrow down papers according to PDF availability, year of publishing, document type, and affiliated institution. Moreover, you can sort the results based on the publishing date, citation count, and relevance.
Assess credibility of papers quickly
When doing the literature review, it is critical to establish the quality of your sources. They form the foundation of your research. SciSpace Discover helps you assess the quality of a source by providing an overview of its references, citations, and performance metrics.
Get the complete picture in no time
SciSpace Discover’s personalized suggestion engine helps you stay on course and get the complete picture of the topic from one place. Every time you visit an article page, it provides you links to related papers. Besides that, it helps you understand what’s trending, who are the top authors, and who are the leading publishers on a topic.
Make referring sources super easy
To ensure you don't lose track of your sources, you must start noting down your references when doing the literature review. SciSpace Discover makes this step effortless. Click the 'cite' button on an article page, and you will receive preloaded citation text in multiple styles — all you've to do is copy-paste it into your manuscript.
Final tips on how to write a literature review
A massive chunk of time and effort is required to write a good literature review. But, if you go about it systematically, you'll be able to save a ton of time and build a solid foundation for your research.
We hope this guide has helped you answer several key questions you have about writing literature reviews.
Would you like to explore SciSpace Discover and kick off your literature search right away? You can get started here .
Frequently Asked Questions (FAQs)
1. how to start a literature review.
• What questions do you want to answer?
• What sources do you need to answer these questions?
• What information do these sources contain?
• How can you use this information to answer your questions?
2. What to include in a literature review?
• A brief background of the problem or issue
• What has previously been done to address the problem or issue
• A description of what you will do in your project
• How this study will contribute to research on the subject
3. Why literature review is important?
The literature review is an important part of any research project because it allows the writer to look at previous studies on a topic and determine existing gaps in the literature, as well as what has already been done. It will also help them to choose the most appropriate method for their own study.
4. How to cite a literature review in APA format?
To cite a literature review in APA style, you need to provide the author's name, the title of the article, and the year of publication. For example: Patel, A. B., & Stokes, G. S. (2012). The relationship between personality and intelligence: A meta-analysis of longitudinal research. Personality and Individual Differences, 53(1), 16-21
5. What are the components of a literature review?
• A brief introduction to the topic, including its background and context. The introduction should also include a rationale for why the study is being conducted and what it will accomplish.
• A description of the methodologies used in the study. This can include information about data collection methods, sample size, and statistical analyses.
• A presentation of the findings in an organized format that helps readers follow along with the author's conclusions.
6. What are common errors in writing literature review?
• Not spending enough time to critically evaluate the relevance of resources, observations and conclusions.
• Totally relying on secondary data while ignoring primary data.
• Letting your personal bias seep into your interpretation of existing literature.
• No detailed explanation of the procedure to discover and identify an appropriate literature review.
7. What are the 5 C's of writing literature review?
• Cite - the sources you utilized and referenced in your research.
• Compare - existing arguments, hypotheses, methodologies, and conclusions found in the knowledge base.
• Contrast - the arguments, topics, methodologies, approaches, and disputes that may be found in the literature.
• Critique - the literature and describe the ideas and opinions you find more convincing and why.
• Connect - the various studies you reviewed in your research.
8. How many sources should a literature review have?
When it is just a chapter, sources should equal the total number of pages in your article's body. if it is a self-contained paper in itself, you need at least three times as many sources as there are pages in your work.
9. Can literature review have diagrams?
• To represent an abstract idea or concept
• To explain the steps of a process or procedure
• To help readers understand the relationships between different concepts
10. How old should sources be in a literature review?
Sources for a literature review should be as current as possible or not older than ten years. The only exception to this rule is if you are reviewing a historical topic and need to use older sources.
11. What are the types of literature review?
• Argumentative review
• Integrative review
• Methodological review
• Systematic review
• Meta-analysis review
• Historical review
• Theoretical review
• Scoping review
• State-of-the-Art review
12. Is a literature review mandatory?
Yes. Literature review is a mandatory part of any research project. It is a critical step in the process that allows you to establish the scope of your research, and provide a background for the rest of your work.
But before you go,
- Six Online Tools for Easy Literature Review
- Evaluating literature review: systematic vs. scoping reviews
- Systematic Approaches to a Successful Literature Review
- Writing Integrative Literature Reviews: Guidelines and Examples
You might also like

Consensus GPT vs. SciSpace GPT: Choose the Best GPT for Research

Literature Review and Theoretical Framework: Understanding the Differences

Types of Essays in Academic Writing - Quick Guide (2024)
- USC Libraries
- Research Guides
Organizing Your Social Sciences Research Paper
- 5. The Literature Review
- Purpose of Guide
- Design Flaws to Avoid
- Independent and Dependent Variables
- Glossary of Research Terms
- Reading Research Effectively
- Narrowing a Topic Idea
- Broadening a Topic Idea
- Extending the Timeliness of a Topic Idea
- Academic Writing Style
- Applying Critical Thinking
- Choosing a Title
- Making an Outline
- Paragraph Development
- Research Process Video Series
- Executive Summary
- The C.A.R.S. Model
- Background Information
- The Research Problem/Question
- Theoretical Framework
- Citation Tracking
- Content Alert Services
- Evaluating Sources
- Primary Sources
- Secondary Sources
- Tiertiary Sources
- Scholarly vs. Popular Publications
- Qualitative Methods
- Quantitative Methods
- Insiderness
- Using Non-Textual Elements
- Limitations of the Study
- Common Grammar Mistakes
- Writing Concisely
- Avoiding Plagiarism
- Footnotes or Endnotes?
- Further Readings
- Generative AI and Writing
- USC Libraries Tutorials and Other Guides
- Bibliography
A literature review surveys prior research published in books, scholarly articles, and any other sources relevant to a particular issue, area of research, or theory, and by so doing, provides a description, summary, and critical evaluation of these works in relation to the research problem being investigated. Literature reviews are designed to provide an overview of sources you have used in researching a particular topic and to demonstrate to your readers how your research fits within existing scholarship about the topic.
Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper . Fourth edition. Thousand Oaks, CA: SAGE, 2014.
Importance of a Good Literature Review
A literature review may consist of simply a summary of key sources, but in the social sciences, a literature review usually has an organizational pattern and combines both summary and synthesis, often within specific conceptual categories . A summary is a recap of the important information of the source, but a synthesis is a re-organization, or a reshuffling, of that information in a way that informs how you are planning to investigate a research problem. The analytical features of a literature review might:
- Give a new interpretation of old material or combine new with old interpretations,
- Trace the intellectual progression of the field, including major debates,
- Depending on the situation, evaluate the sources and advise the reader on the most pertinent or relevant research, or
- Usually in the conclusion of a literature review, identify where gaps exist in how a problem has been researched to date.
Given this, the purpose of a literature review is to:
- Place each work in the context of its contribution to understanding the research problem being studied.
- Describe the relationship of each work to the others under consideration.
- Identify new ways to interpret prior research.
- Reveal any gaps that exist in the literature.
- Resolve conflicts amongst seemingly contradictory previous studies.
- Identify areas of prior scholarship to prevent duplication of effort.
- Point the way in fulfilling a need for additional research.
- Locate your own research within the context of existing literature [very important].
Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper. 2nd ed. Thousand Oaks, CA: Sage, 2005; Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1998; Jesson, Jill. Doing Your Literature Review: Traditional and Systematic Techniques . Los Angeles, CA: SAGE, 2011; Knopf, Jeffrey W. "Doing a Literature Review." PS: Political Science and Politics 39 (January 2006): 127-132; Ridley, Diana. The Literature Review: A Step-by-Step Guide for Students . 2nd ed. Los Angeles, CA: SAGE, 2012.
Types of Literature Reviews
It is important to think of knowledge in a given field as consisting of three layers. First, there are the primary studies that researchers conduct and publish. Second are the reviews of those studies that summarize and offer new interpretations built from and often extending beyond the primary studies. Third, there are the perceptions, conclusions, opinion, and interpretations that are shared informally among scholars that become part of the body of epistemological traditions within the field.
In composing a literature review, it is important to note that it is often this third layer of knowledge that is cited as "true" even though it often has only a loose relationship to the primary studies and secondary literature reviews. Given this, while literature reviews are designed to provide an overview and synthesis of pertinent sources you have explored, there are a number of approaches you could adopt depending upon the type of analysis underpinning your study.
Argumentative Review This form examines literature selectively in order to support or refute an argument, deeply embedded assumption, or philosophical problem already established in the literature. The purpose is to develop a body of literature that establishes a contrarian viewpoint. Given the value-laden nature of some social science research [e.g., educational reform; immigration control], argumentative approaches to analyzing the literature can be a legitimate and important form of discourse. However, note that they can also introduce problems of bias when they are used to make summary claims of the sort found in systematic reviews [see below].
Integrative Review Considered a form of research that reviews, critiques, and synthesizes representative literature on a topic in an integrated way such that new frameworks and perspectives on the topic are generated. The body of literature includes all studies that address related or identical hypotheses or research problems. A well-done integrative review meets the same standards as primary research in regard to clarity, rigor, and replication. This is the most common form of review in the social sciences.
Historical Review Few things rest in isolation from historical precedent. Historical literature reviews focus on examining research throughout a period of time, often starting with the first time an issue, concept, theory, phenomena emerged in the literature, then tracing its evolution within the scholarship of a discipline. The purpose is to place research in a historical context to show familiarity with state-of-the-art developments and to identify the likely directions for future research.
Methodological Review A review does not always focus on what someone said [findings], but how they came about saying what they say [method of analysis]. Reviewing methods of analysis provides a framework of understanding at different levels [i.e. those of theory, substantive fields, research approaches, and data collection and analysis techniques], how researchers draw upon a wide variety of knowledge ranging from the conceptual level to practical documents for use in fieldwork in the areas of ontological and epistemological consideration, quantitative and qualitative integration, sampling, interviewing, data collection, and data analysis. This approach helps highlight ethical issues which you should be aware of and consider as you go through your own study.
Systematic Review This form consists of an overview of existing evidence pertinent to a clearly formulated research question, which uses pre-specified and standardized methods to identify and critically appraise relevant research, and to collect, report, and analyze data from the studies that are included in the review. The goal is to deliberately document, critically evaluate, and summarize scientifically all of the research about a clearly defined research problem . Typically it focuses on a very specific empirical question, often posed in a cause-and-effect form, such as "To what extent does A contribute to B?" This type of literature review is primarily applied to examining prior research studies in clinical medicine and allied health fields, but it is increasingly being used in the social sciences.
Theoretical Review The purpose of this form is to examine the corpus of theory that has accumulated in regard to an issue, concept, theory, phenomena. The theoretical literature review helps to establish what theories already exist, the relationships between them, to what degree the existing theories have been investigated, and to develop new hypotheses to be tested. Often this form is used to help establish a lack of appropriate theories or reveal that current theories are inadequate for explaining new or emerging research problems. The unit of analysis can focus on a theoretical concept or a whole theory or framework.
NOTE: Most often the literature review will incorporate some combination of types. For example, a review that examines literature supporting or refuting an argument, assumption, or philosophical problem related to the research problem will also need to include writing supported by sources that establish the history of these arguments in the literature.
Baumeister, Roy F. and Mark R. Leary. "Writing Narrative Literature Reviews." Review of General Psychology 1 (September 1997): 311-320; Mark R. Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper . 2nd ed. Thousand Oaks, CA: Sage, 2005; Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1998; Kennedy, Mary M. "Defining a Literature." Educational Researcher 36 (April 2007): 139-147; Petticrew, Mark and Helen Roberts. Systematic Reviews in the Social Sciences: A Practical Guide . Malden, MA: Blackwell Publishers, 2006; Torracro, Richard. "Writing Integrative Literature Reviews: Guidelines and Examples." Human Resource Development Review 4 (September 2005): 356-367; Rocco, Tonette S. and Maria S. Plakhotnik. "Literature Reviews, Conceptual Frameworks, and Theoretical Frameworks: Terms, Functions, and Distinctions." Human Ressource Development Review 8 (March 2008): 120-130; Sutton, Anthea. Systematic Approaches to a Successful Literature Review . Los Angeles, CA: Sage Publications, 2016.
Structure and Writing Style
I. Thinking About Your Literature Review
The structure of a literature review should include the following in support of understanding the research problem :
- An overview of the subject, issue, or theory under consideration, along with the objectives of the literature review,
- Division of works under review into themes or categories [e.g. works that support a particular position, those against, and those offering alternative approaches entirely],
- An explanation of how each work is similar to and how it varies from the others,
- Conclusions as to which pieces are best considered in their argument, are most convincing of their opinions, and make the greatest contribution to the understanding and development of their area of research.
The critical evaluation of each work should consider :
- Provenance -- what are the author's credentials? Are the author's arguments supported by evidence [e.g. primary historical material, case studies, narratives, statistics, recent scientific findings]?
- Methodology -- were the techniques used to identify, gather, and analyze the data appropriate to addressing the research problem? Was the sample size appropriate? Were the results effectively interpreted and reported?
- Objectivity -- is the author's perspective even-handed or prejudicial? Is contrary data considered or is certain pertinent information ignored to prove the author's point?
- Persuasiveness -- which of the author's theses are most convincing or least convincing?
- Validity -- are the author's arguments and conclusions convincing? Does the work ultimately contribute in any significant way to an understanding of the subject?
II. Development of the Literature Review
Four Basic Stages of Writing 1. Problem formulation -- which topic or field is being examined and what are its component issues? 2. Literature search -- finding materials relevant to the subject being explored. 3. Data evaluation -- determining which literature makes a significant contribution to the understanding of the topic. 4. Analysis and interpretation -- discussing the findings and conclusions of pertinent literature.
Consider the following issues before writing the literature review: Clarify If your assignment is not specific about what form your literature review should take, seek clarification from your professor by asking these questions: 1. Roughly how many sources would be appropriate to include? 2. What types of sources should I review (books, journal articles, websites; scholarly versus popular sources)? 3. Should I summarize, synthesize, or critique sources by discussing a common theme or issue? 4. Should I evaluate the sources in any way beyond evaluating how they relate to understanding the research problem? 5. Should I provide subheadings and other background information, such as definitions and/or a history? Find Models Use the exercise of reviewing the literature to examine how authors in your discipline or area of interest have composed their literature review sections. Read them to get a sense of the types of themes you might want to look for in your own research or to identify ways to organize your final review. The bibliography or reference section of sources you've already read, such as required readings in the course syllabus, are also excellent entry points into your own research. Narrow the Topic The narrower your topic, the easier it will be to limit the number of sources you need to read in order to obtain a good survey of relevant resources. Your professor will probably not expect you to read everything that's available about the topic, but you'll make the act of reviewing easier if you first limit scope of the research problem. A good strategy is to begin by searching the USC Libraries Catalog for recent books about the topic and review the table of contents for chapters that focuses on specific issues. You can also review the indexes of books to find references to specific issues that can serve as the focus of your research. For example, a book surveying the history of the Israeli-Palestinian conflict may include a chapter on the role Egypt has played in mediating the conflict, or look in the index for the pages where Egypt is mentioned in the text. Consider Whether Your Sources are Current Some disciplines require that you use information that is as current as possible. This is particularly true in disciplines in medicine and the sciences where research conducted becomes obsolete very quickly as new discoveries are made. However, when writing a review in the social sciences, a survey of the history of the literature may be required. In other words, a complete understanding the research problem requires you to deliberately examine how knowledge and perspectives have changed over time. Sort through other current bibliographies or literature reviews in the field to get a sense of what your discipline expects. You can also use this method to explore what is considered by scholars to be a "hot topic" and what is not.
III. Ways to Organize Your Literature Review
Chronology of Events If your review follows the chronological method, you could write about the materials according to when they were published. This approach should only be followed if a clear path of research building on previous research can be identified and that these trends follow a clear chronological order of development. For example, a literature review that focuses on continuing research about the emergence of German economic power after the fall of the Soviet Union. By Publication Order your sources by publication chronology, then, only if the order demonstrates a more important trend. For instance, you could order a review of literature on environmental studies of brown fields if the progression revealed, for example, a change in the soil collection practices of the researchers who wrote and/or conducted the studies. Thematic [“conceptual categories”] A thematic literature review is the most common approach to summarizing prior research in the social and behavioral sciences. Thematic reviews are organized around a topic or issue, rather than the progression of time, although the progression of time may still be incorporated into a thematic review. For example, a review of the Internet’s impact on American presidential politics could focus on the development of online political satire. While the study focuses on one topic, the Internet’s impact on American presidential politics, it would still be organized chronologically reflecting technological developments in media. The difference in this example between a "chronological" and a "thematic" approach is what is emphasized the most: themes related to the role of the Internet in presidential politics. Note that more authentic thematic reviews tend to break away from chronological order. A review organized in this manner would shift between time periods within each section according to the point being made. Methodological A methodological approach focuses on the methods utilized by the researcher. For the Internet in American presidential politics project, one methodological approach would be to look at cultural differences between the portrayal of American presidents on American, British, and French websites. Or the review might focus on the fundraising impact of the Internet on a particular political party. A methodological scope will influence either the types of documents in the review or the way in which these documents are discussed.
Other Sections of Your Literature Review Once you've decided on the organizational method for your literature review, the sections you need to include in the paper should be easy to figure out because they arise from your organizational strategy. In other words, a chronological review would have subsections for each vital time period; a thematic review would have subtopics based upon factors that relate to the theme or issue. However, sometimes you may need to add additional sections that are necessary for your study, but do not fit in the organizational strategy of the body. What other sections you include in the body is up to you. However, only include what is necessary for the reader to locate your study within the larger scholarship about the research problem.
Here are examples of other sections, usually in the form of a single paragraph, you may need to include depending on the type of review you write:
- Current Situation : Information necessary to understand the current topic or focus of the literature review.
- Sources Used : Describes the methods and resources [e.g., databases] you used to identify the literature you reviewed.
- History : The chronological progression of the field, the research literature, or an idea that is necessary to understand the literature review, if the body of the literature review is not already a chronology.
- Selection Methods : Criteria you used to select (and perhaps exclude) sources in your literature review. For instance, you might explain that your review includes only peer-reviewed [i.e., scholarly] sources.
- Standards : Description of the way in which you present your information.
- Questions for Further Research : What questions about the field has the review sparked? How will you further your research as a result of the review?
IV. Writing Your Literature Review
Once you've settled on how to organize your literature review, you're ready to write each section. When writing your review, keep in mind these issues.
Use Evidence A literature review section is, in this sense, just like any other academic research paper. Your interpretation of the available sources must be backed up with evidence [citations] that demonstrates that what you are saying is valid. Be Selective Select only the most important points in each source to highlight in the review. The type of information you choose to mention should relate directly to the research problem, whether it is thematic, methodological, or chronological. Related items that provide additional information, but that are not key to understanding the research problem, can be included in a list of further readings . Use Quotes Sparingly Some short quotes are appropriate if you want to emphasize a point, or if what an author stated cannot be easily paraphrased. Sometimes you may need to quote certain terminology that was coined by the author, is not common knowledge, or taken directly from the study. Do not use extensive quotes as a substitute for using your own words in reviewing the literature. Summarize and Synthesize Remember to summarize and synthesize your sources within each thematic paragraph as well as throughout the review. Recapitulate important features of a research study, but then synthesize it by rephrasing the study's significance and relating it to your own work and the work of others. Keep Your Own Voice While the literature review presents others' ideas, your voice [the writer's] should remain front and center. For example, weave references to other sources into what you are writing but maintain your own voice by starting and ending the paragraph with your own ideas and wording. Use Caution When Paraphrasing When paraphrasing a source that is not your own, be sure to represent the author's information or opinions accurately and in your own words. Even when paraphrasing an author’s work, you still must provide a citation to that work.
V. Common Mistakes to Avoid
These are the most common mistakes made in reviewing social science research literature.
- Sources in your literature review do not clearly relate to the research problem;
- You do not take sufficient time to define and identify the most relevant sources to use in the literature review related to the research problem;
- Relies exclusively on secondary analytical sources rather than including relevant primary research studies or data;
- Uncritically accepts another researcher's findings and interpretations as valid, rather than examining critically all aspects of the research design and analysis;
- Does not describe the search procedures that were used in identifying the literature to review;
- Reports isolated statistical results rather than synthesizing them in chi-squared or meta-analytic methods; and,
- Only includes research that validates assumptions and does not consider contrary findings and alternative interpretations found in the literature.
Cook, Kathleen E. and Elise Murowchick. “Do Literature Review Skills Transfer from One Course to Another?” Psychology Learning and Teaching 13 (March 2014): 3-11; Fink, Arlene. Conducting Research Literature Reviews: From the Internet to Paper . 2nd ed. Thousand Oaks, CA: Sage, 2005; Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1998; Jesson, Jill. Doing Your Literature Review: Traditional and Systematic Techniques . London: SAGE, 2011; Literature Review Handout. Online Writing Center. Liberty University; Literature Reviews. The Writing Center. University of North Carolina; Onwuegbuzie, Anthony J. and Rebecca Frels. Seven Steps to a Comprehensive Literature Review: A Multimodal and Cultural Approach . Los Angeles, CA: SAGE, 2016; Ridley, Diana. The Literature Review: A Step-by-Step Guide for Students . 2nd ed. Los Angeles, CA: SAGE, 2012; Randolph, Justus J. “A Guide to Writing the Dissertation Literature Review." Practical Assessment, Research, and Evaluation. vol. 14, June 2009; Sutton, Anthea. Systematic Approaches to a Successful Literature Review . Los Angeles, CA: Sage Publications, 2016; Taylor, Dena. The Literature Review: A Few Tips On Conducting It. University College Writing Centre. University of Toronto; Writing a Literature Review. Academic Skills Centre. University of Canberra.
Writing Tip
Break Out of Your Disciplinary Box!
Thinking interdisciplinarily about a research problem can be a rewarding exercise in applying new ideas, theories, or concepts to an old problem. For example, what might cultural anthropologists say about the continuing conflict in the Middle East? In what ways might geographers view the need for better distribution of social service agencies in large cities than how social workers might study the issue? You don’t want to substitute a thorough review of core research literature in your discipline for studies conducted in other fields of study. However, particularly in the social sciences, thinking about research problems from multiple vectors is a key strategy for finding new solutions to a problem or gaining a new perspective. Consult with a librarian about identifying research databases in other disciplines; almost every field of study has at least one comprehensive database devoted to indexing its research literature.
Frodeman, Robert. The Oxford Handbook of Interdisciplinarity . New York: Oxford University Press, 2010.
Another Writing Tip
Don't Just Review for Content!
While conducting a review of the literature, maximize the time you devote to writing this part of your paper by thinking broadly about what you should be looking for and evaluating. Review not just what scholars are saying, but how are they saying it. Some questions to ask:
- How are they organizing their ideas?
- What methods have they used to study the problem?
- What theories have been used to explain, predict, or understand their research problem?
- What sources have they cited to support their conclusions?
- How have they used non-textual elements [e.g., charts, graphs, figures, etc.] to illustrate key points?
When you begin to write your literature review section, you'll be glad you dug deeper into how the research was designed and constructed because it establishes a means for developing more substantial analysis and interpretation of the research problem.
Hart, Chris. Doing a Literature Review: Releasing the Social Science Research Imagination . Thousand Oaks, CA: Sage Publications, 1 998.
Yet Another Writing Tip
When Do I Know I Can Stop Looking and Move On?
Here are several strategies you can utilize to assess whether you've thoroughly reviewed the literature:
- Look for repeating patterns in the research findings . If the same thing is being said, just by different people, then this likely demonstrates that the research problem has hit a conceptual dead end. At this point consider: Does your study extend current research? Does it forge a new path? Or, does is merely add more of the same thing being said?
- Look at sources the authors cite to in their work . If you begin to see the same researchers cited again and again, then this is often an indication that no new ideas have been generated to address the research problem.
- Search Google Scholar to identify who has subsequently cited leading scholars already identified in your literature review [see next sub-tab]. This is called citation tracking and there are a number of sources that can help you identify who has cited whom, particularly scholars from outside of your discipline. Here again, if the same authors are being cited again and again, this may indicate no new literature has been written on the topic.
Onwuegbuzie, Anthony J. and Rebecca Frels. Seven Steps to a Comprehensive Literature Review: A Multimodal and Cultural Approach . Los Angeles, CA: Sage, 2016; Sutton, Anthea. Systematic Approaches to a Successful Literature Review . Los Angeles, CA: Sage Publications, 2016.
- << Previous: Theoretical Framework
- Next: Citation Tracking >>
- Last Updated: Sep 4, 2024 9:40 AM
- URL: https://libguides.usc.edu/writingguide

Literature Reviews
What is a Literature Review?
- Steps for Creating a Literature Review
- Providing Evidence / Critical Analysis
- Challenges when writing a Literature Review
- Systematic Literature Reviews
A literature review is an academic text that surveys, synthesizes, and critically evaluates the existing literature on a specific topic. It is typically required for theses, dissertations, or long reports and serves several key purposes:
- Surveying the Literature : It involves a comprehensive search and examination of relevant academic books, journal articles, and other sources related to the chosen topic.
- Synthesizing Information : The literature review summarizes and organizes the information found in the literature, often identifying patterns, themes, and gaps in the current knowledge.
- Critical Analysis : It critically analyzes the collected information, highlighting limitations, gaps, and areas of controversy, and suggests directions for future research.
- Establishing Context : It places the current research within the broader context of the field, demonstrating how the new research builds on or diverges from previous studies.
Types of Literature Reviews
Literature reviews can take various forms, including:
- Narrative Reviews : These provide a qualitative summary of the literature and are often used to give a broad overview of a topic. They may be less structured and more subjective, focusing on synthesizing the literature to support a particular viewpoint.
- Systematic Reviews : These are more rigorous and structured, following a specific methodology to identify, evaluate, and synthesize all relevant studies on a particular question. They aim to minimize bias and provide a comprehensive summary of the existing evidence.
- Integrative Reviews : Similar to systematic reviews, but they aim to generate new knowledge by integrating findings from different studies to develop new theories or frameworks.
Importance of Literature Reviews
- Foundation for Research : They provide a solid background for new research projects, helping to justify the research question and methodology.
Identifying Gaps : Literature reviews highlight areas where knowledge is lacking, guiding future research efforts.
- Building Credibility : Demonstrating familiarity with existing research enhances the credibility of the researcher and their work.
In summary, a literature review is a critical component of academic research that helps to frame the current state of knowledge, identify gaps, and provide a basis for new research.
The research, the body of current literature, and the particular objectives should all influence the structure of a literature review. It is also critical to remember that creating a literature review is an ongoing process - as one reads and analyzes the literature, one's understanding may change, which could require rearranging the literature review.
Paré, G. and Kitsiou, S. (2017) 'Methods for Literature Reviews' , in: Lau, F. and Kuziemsky, C. (eds.) Handbook of eHealth evaluation: an evidence-based approach . Victoria (BC): University of Victoria.
Perplexity AI (2024) Perplexity AI response to Kathy Neville, 31 July.
Royal Literary Fund (2024) The structure of a literature review. Available at: https://www.rlf.org.uk/resources/the-structure-of-a-literature-review/ (Accessed: 23 July 2024).
Library Services for Undergraduate Research (2024) Literature review: a definition . Available at: https://libguides.wustl.edu/our?p=302677 (Accessed: 31 July 2024).
Further Reading:
Methods for Literature Reviews
Literature Review (The University of Edinburgh)
Literature Reviews (University of Sheffield)
- How to Write a Literature Review Paper? Wee, Bert Van ; Banister, David ISBN: 0144-1647
- Next: Steps for Creating a Literature Review >>
- Last Updated: Sep 4, 2024 11:43 AM
- URL: https://library.lsbu.ac.uk/literaturereviews
A systematic literature review of deep learning-based text summarization: : Techniques, input representation, training strategies, mechanisms, datasets, evaluation, and challenges
New citation alert added.
This alert has been successfully added and will be sent to:
You will be notified whenever a record that you have chosen has been cited.
To manage your alert preferences, click on the button below.
New Citation Alert!
Please log in to your account
Information & Contributors
Bibliometrics & citations, view options, recommendations, optimal features set for extractive automatic text summarization.
The goal of text summarization is to reduce the size of the text while preserving its important information and overall meaning. With the availability of internet, data is growing leaps and bounds and it is practically impossible summarizing all this ...
RankSum—An unsupervised extractive text summarization based on rank fusion
In this paper, we propose Ranksum, an approach for extractive text summarization of single documents based on the rank fusion of four multi-dimensional sentence features extracted for each sentence: topic information, semantic content, ...
Display Omitted
- A unified summarization framework with multi-dimensional sentence features.
An Experimental Investigation on Unsupervised Text Summarization for Customer Reviews
People generally turn to websites such as Yelp to find reviews for the food/restaurant before trying it first-hand. However, some reviews are so long and ambiguous that users get confused about whether the review appreciates or disparages the ...
Information
Published in.
Pergamon Press, Inc.
United States
Publication History
Author tags.
- Deep learning
- Text summarization
- Abstractive
- Review-article
Contributors
Other metrics, bibliometrics, article metrics.
- 0 Total Citations
- 0 Total Downloads
- Downloads (Last 12 months) 0
- Downloads (Last 6 weeks) 0
View options
Login options.
Check if you have access through your login credentials or your institution to get full access on this article.
Full Access
Share this publication link.
Copying failed.
Share on social media
Affiliations, export citations.
- Please download or close your previous search result export first before starting a new bulk export. Preview is not available. By clicking download, a status dialog will open to start the export process. The process may take a few minutes but once it finishes a file will be downloadable from your browser. You may continue to browse the DL while the export process is in progress. Download
- Download citation
- Copy citation
We are preparing your search results for download ...
We will inform you here when the file is ready.
Your file of search results citations is now ready.
Your search export query has expired. Please try again.
This week: the arXiv Accessibility Forum
Help | Advanced Search
Computer Science > Machine Learning
Title: multimodal methods for analyzing learning and training environments: a systematic literature review.
Abstract: Recent technological advancements have enhanced our ability to collect and analyze rich multimodal data (e.g., speech, video, and eye gaze) to better inform learning and training experiences. While previous reviews have focused on parts of the multimodal pipeline (e.g., conceptual models and data fusion), a comprehensive literature review on the methods informing multimodal learning and training environments has not been conducted. This literature review provides an in-depth analysis of research methods in these environments, proposing a taxonomy and framework that encapsulates recent methodological advances in this field and characterizes the multimodal domain in terms of five modality groups: Natural Language, Video, Sensors, Human-Centered, and Environment Logs. We introduce a novel data fusion category -- mid fusion -- and a graph-based technique for refining literature reviews, termed citation graph pruning. Our analysis reveals that leveraging multiple modalities offers a more holistic understanding of the behaviors and outcomes of learners and trainees. Even when multimodality does not enhance predictive accuracy, it often uncovers patterns that contextualize and elucidate unimodal data, revealing subtleties that a single modality may miss. However, there remains a need for further research to bridge the divide between multimodal learning and training studies and foundational AI research.
| Comments: | Submitted to ACM Computing Surveys. Currently under review |
| Subjects: | Machine Learning (cs.LG); Multimedia (cs.MM) |
| Cite as: | [cs.LG] |
| (or [cs.LG] for this version) | |
| Focus to learn more arXiv-issued DOI via DataCite |
Submission history
Access paper:.
- HTML (experimental)
- Other Formats
References & Citations
- Google Scholar
- Semantic Scholar
BibTeX formatted citation
Bibliographic and Citation Tools
Code, data and media associated with this article, recommenders and search tools.
- Institution
arXivLabs: experimental projects with community collaborators
arXivLabs is a framework that allows collaborators to develop and share new arXiv features directly on our website.
Both individuals and organizations that work with arXivLabs have embraced and accepted our values of openness, community, excellence, and user data privacy. arXiv is committed to these values and only works with partners that adhere to them.
Have an idea for a project that will add value for arXiv's community? Learn more about arXivLabs .
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- PMC11142523

A systematic review of barriers and facilitators to antenatal screening for HIV, syphilis or hepatitis B in Asia: Perspectives of pregnant women, their relatives and health care providers
Lucie sabin.
Institute for Global Health, University College London, London, United Kingdom
Hassan Haghparast-Bidgoli
Faith miller, naomi saville, associated data.
All relevant data are within the manuscript and its Supporting Information files.
Despite improvements, the prevalence of HIV, syphilis, and hepatitis B remains high in Asia. These sexually transmitted infections (STIs) can be transmitted from infected mothers to their children. Antenatal screening and treatment are effective interventions to prevent mother-to-child transmission (MTCT), but coverage of antenatal screening remains low. Understanding factors influencing antenatal screening is essential to increase its uptake and design effective interventions. This systematic literature review aims to investigate barriers and facilitators to antenatal screening for HIV, syphilis, and hepatitis B in Asia.
We conducted a systematic review by searching Ovid (MEDLINE, Embase, PsycINFO), Scopus, Global Index Medicus and Web of Science for published articles between January 2000 and June 2023, and screening abstracts and full articles. Eligible studies include peer-reviewed journal articles of quantitative, qualitative and mixed-method studies that explored factors influencing the use of antenatal screening for HIV, syphilis or hepatitis B in Asia. We extracted key information including study characteristics, sample, aim, identified barriers and facilitators to screening. We conducted a narrative synthesis to summarise the findings and presented barriers and facilitators following Andersen’s conceptual model.
The literature search revealed 23 articles suitable for inclusion, 19 used quantitative methods, 3 qualitative and one mixed method. We found only three studies on syphilis screening and one on hepatitis B. The analysis demonstrates that antenatal screening for HIV in Asia is influenced by many barriers and facilitators including (1) predisposing characteristics of pregnant women (age, education level, knowledge) (2) enabling factors (wealth, place of residence, husband support, health facilities characteristics, health workers support and training) (3) need factors of pregnant women (risk perception, perceived benefits of screening).
Knowledge of identified barriers to antenatal screening may support implementation of appropriate interventions to prevent MTCT and help countries achieve Sustainable Development Goals’ targets for HIV and STIs.
Introduction
Human immunodeficiency virus (HIV), syphilis and hepatitis B are sexually transmitted infections (STIs) that, if left undiagnosed and untreated, can lead to serious complications and death. Despite improvements in the last decade, their prevalence remains high in Asia [ 1 , 2 ]. In 2017, 5.2 million people were living with HIV in the Asia Pacific region [ 3 ] and 123,000 people died from HIV-related causes in 2021 [ 4 ]. The regional prevalence of HIV was 0.2% [ 4 ]. In 2012, an estimated 1.8 million women were infected with syphilis in the South-East Asia region [ 5 ] and 39 million people with hepatitis B with a prevalence of 2.0% [ 6 ].
These STIs can be transmitted from infected mothers to their children during pregnancy and childbirth, resulting in significant morbidity and mortality. The rate of mother-to-child transmission of HIV in Asia and the Pacific is relatively high, at 17%, among the estimated 61,000 women living with HIV who gave birth in the region in 2017 [ 3 ] and 1.3 million pregnant women are at risk of transmitting HBV to their newborns each year [ 7 ]. The global number of adverse pregnancy events attributable to maternal syphilis infection was estimated to be 52,307 in the South-East Asia Region and 13,472 in the Western Pacific Region [ 8 ].
Mother-to-child transmission (MTCT), also called vertical transmission, can be prevented with simple and effective interventions, including antenatal screening and treatment, prevention of male-to-female transmission during sexual intercourse, and improving community awareness. Antenatal screening is an essential tool to enable women to find out if they are infected and to take the necessary steps to access preventive treatment if they test positive in order to avoid MTCT [ 9 ]. Since 2010, an estimated 7,400 new HIV infections among children in the Asia Pacific region were averted because of interventions aimed at reducing the MTCT of HIV [ 3 ]. However, due to limited availability and access to these interventions [ 10 ], antenatal screening for STIs in Asia remains low [ 11 ]. Only three of the 17 reporting countries in the Asia-Pacific region met the global target of over 95% coverage for knowledge of HIV status among women receiving ANC in 2017 and six countries (Bangladesh, Timor-Leste, Papuz New Guinea, Lao People’s Democratic Republic, Indonesia, Singapore) reported coverage below 40% [ 11 ]. Only thirteen countries currently out of 17 countries have a policy of screening for hepatitis B during pregnancy, and very little data on hepatitis B screening coverage is currently available [ 10 ]. Most Asian countries also have no data on syphilis screening for pregnant women. Of the 28 countries in Asia and Pacific regions (according to WHO definitions of regions) reporting antenatal screening coverage for syphilis between 2010 and 2017, four countries reported coverage between 20% and 49% (India, Myanmar, Vanuatu, Papua New Guinea) and three reported coverage below 5% (Afghanistan, Indonesia, Solomon Islands) [ 11 ]. Yet unknowingly infected people can transmit infections to their sexual partners and infected women to their children through MTCT. This also prevents them from accessing timely treatment leading to long-term complications that generate significant costs for the health system. In addition, low uptake of STIs screening services can exacerbate existing health disparities, with vulnerable populations, such as marginalised communities or migrant populations, facing additional barriers to accessing screening services.
To guide a path towards triple elimination of MTCT of HIV, syphilis, and hepatitis B in Asia and the Pacific, the WHO developed a regional framework [ 10 ]. This framework aims to eliminate these three infections in newborns and infants by 2030 in Asia. The key recommendations emphasise an integrated approach to triple elimination, recognising the interconnectedness of the three diseases and the potential for resource optimisation and highlights the importance of strengthening health systems to effectively deliver comprehensive services and achieve universal health coverage. The framework focuses on building capacity, improving laboratory and diagnostic services, ensuring a reliable supply chain for medicines and commodities, and improving reporting systems. It recognises the need for collaboration between different sectors beyond the health sector and the importance of sustainable financing mechanisms to support the implementation of elimination programmes. Meanwhile, it encourages the participation of women living with HIV, women affected by syphilis, and mothers with hepatitis B, men and communities in the design, implementation, and evaluation of programmes and policies.
Understanding barriers and facilitators influencing antenatal screening for STIs is essential to design effective screening interventions. The information will also be useful to help countries to achieve a key health target of the Sustainable Development Goals (SDGs), i.e., “end the epidemics of AIDS, tuberculosis, malaria and neglected tropical diseases and combat hepatitis, water-borne diseases, and other communicable diseases by 2030”. A systematic review conducted by Blackstone et al. [ 12 ] investigated the barriers and facilitators to routine antenatal HIV screening in sub-Saharan Africa, using literature published between 2000 and 2015. They identified the fear of the screening results, perceived stigma towards HIV-positive people, fear of the partner’s reaction in case of a positive test result, and perceived partner disapproval of the test as barriers to antenatal HIV screening. A high level of education, good knowledge of MTCT and HIV, and partner involvement in antenatal care were favourable factors for screening. Health system and provider issues affected the acceptance of antenatal screening. Good patient-provider communication, counselling to improve knowledge of pregnant women of the benefits of screening through counselling, and the perception that HIV screening is mandatory were facilitators to screening.
Barriers are likely to change over time, as societies evolve, beliefs change, or targeted interventions are put in place. There is no literature review summarising the evidence on barriers and facilitators to antenatal screening for HIV, syphilis, and hepatitis B in the Asian context. Factors affecting screening are likely to be different from those in the African context due to cultural and contextual differences. This hinders the development of targeted strategies and interventions to overcome barriers and improve the effectiveness of antenatal screening programmes. It also limits the application of the WHO framework towards triple elimination of MTCT of HIV, syphilis and hepatitis B. Health care providers in Asia may also lack guidance on how to effectively implement and improve antenatal screening programmes for STIs. Barriers preventing vulnerable communities from accessing screening are not known, which may contribute to disparities in health outcomes, with potentially negative impacts on maternal and child health.
In order to fill this evidence gap, this review aimed to investigate the barriers and facilitators to antenatal screening for HIV, syphilis, or hepatitis B for women in Asia. Its specific objectives were to identify available evidence and underline possible gaps in the research knowledge base surrounding this subject.
Methods and analysis
The review and its reporting comply with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist ( S1 Table ) and the protocol has been published on PROSPERO (registration number CRD42023435483).
Search strategy
We conducted a comprehensive search of electronic databases including Ovid (MEDLINE, Embase, PsycINFO), Scopus, Global Index Medicus, and Web of Science was conducted to identify relevant studies published between 2000 and June 2023. The first search was conducted on 13 December 2021 and repeated on 10 June 2023 by LS. The keyword search was divided into five main groups: “barriers or facilitators”, “antenatal screening”, “HIV or syphilis or hepatitis B”, and “Asian countries”. The finalised search terms were developed through a trial-and-error process for use on Scopus and adapted to the different databases. The full key words used are shown in S1 File .
We used forward and backward citation searching to capture resources either citing or being cited by the included literature and searched the websites of the WHO, the World Bank and UNAIDS for reports.
Inclusion criteria
The eligibility criteria for study inclusion were developed using the acronym SPlDER: S sample; P phenomenon of interest; D design; E evaluation; R research type [ 13 ] ( Table 1 ).
| Pregnant women or women of childbearing age in Asian countries, their family members, health workers and decision-makers (the search term including all the Asian countries as defined by the United Nations is provided in ). | |
| Barriers and facilitators to antenatal screening and factors influencing screening uptake. Barriers were defined as factors discouraging or impeding screening uptake. Facilitators were defined as factors or resources enhancing screening uptake. Factors may also relate to the implementation and effectiveness of antenatal screening. | |
| Primary or secondary research studies, including quantitative, qualitative, and mixed-methods studies. | |
| Antenatal screening programs or interventions related to the screening of HIV, syphilis, or hepatitis B during pregnancy. | |
| Peer-reviewed journal articles in English conducted between 2000 and June 2023. |
Study selection
Following the initial search, LS collated records and uploaded them into Rayyan [ 14 ] to facilitate screening. After removal of duplicates, two independent reviewers (LS and FM) screened titles and abstracts for relevance and assessed full text of potentially relevant article using the inclusion criteria. Those meeting inclusion criteria at full-text screen were included in our results. Any discrepancies were resolved through discussion or consultation with a third reviewer (NS) when needed.
Data extraction
We used a standard form to extract key information including study characteristics (author, year, country, urban/rural setting, diseases considered), study design, sample, aim, identified significant barriers and facilitators to screening (e.g., odds ratios at the 95% confidence interval, p-value < 0.05). We thematically analysed qualitative articles through an iterative process of reading and coding them using Andersen’s framework [ 15 ]. This theoretical framework widely used in literature reviews on healthcare utilisation [ 16 ] provides understanding of how individuals and environmental factors influence health behaviours. The framework categorises predictors of health service use as i) Predisposing characteristics including demographic factors, social structure, and health beliefs that influence health services use. ii) Enabling factors allowing the individual to seek health services if needed. iii) Need factors including perceived needs of healthcare services use.
Quality assessment
LS and FM assessed the quality of included studies using tools appropriate to the study design. The quality of the studies included was evaluated based on Von Elm et al’s [ 17 ] checklist for observational studies and O’Brien et al’s [ 18 ] checklist for qualitative studies. S2 and S3 Tables present the quality appraisal checklists for the considered studies. We scored each paper based on how many checklist items were met. Overall, papers that met over 75% of the checklist items were considered to be of high quality, those meeting 50% to 75% of the checklist were regarded as moderate quality, and those meeting less than 50% poor quality. Because the aim was to describe and synthesise a body of the literature and not determine an effect size, studies were not excluded based on quality.
Data analysis and presentation
Descriptive characteristics of research studies were presented in tables. A narrative synthesis (Popay et al. 2006) was conducted to summarize the findings of the included studies. We did not combine quantitative estimates because of the heterogeneity of approaches and findings. Themes and patterns related to factors influencing screening uptake were identified and analysed and the final set of barriers and facilitators categorised according to Andersen [ 15 ]’s conceptual model.
After the selection process, 23 articles met the eligibility criteria and were included in the review. The PRISMA diagram provides an overview of the selection process ( Fig 1 ).

General study characteristics
Details about the articles included are presented in Table 2 . Most included studies were on HIV screening, one was on syphilis screening [ 19 ], one on HIV and syphilis [ 20 ] and one on HIV, syphilis and hepatitis B [ 21 ]. Eight out of the 23 studies used data collected after 2015 [ 20 , 22 – 28 ]. Six of the studies were conducted in Vietnam, five in India, three in Indonesia, two in Cambodia, and one each in Hong Kong, Mongolia, China, Afghanistan and Thailand. Nineteen of the studies (83%) used quantitative methods, three (15%) used qualitative methods, and one (2%) used mixed methods.
| Citation | Date | Country | Urban/ rural | Disease | Sample | Study type | Aim |
|---|---|---|---|---|---|---|---|
| Dinh [ ] | 2005 | Vietnam | Urban | HIV | 500 pregnant women 18 aged years and older who were first-time antenatal care (ANC) visitors and had never been tested or were unaware of their results | Quantitative | Identify the factors associated with declining HIV antenatal screening and the failure to return for results |
| Nguyen [ ] | 2010 | Vietnam | Urban | HIV | 300 women who had recently delivered | Quantitative | Describe the uptake of antenatal HIV screening |
| Hạnh [ ] | 2011 | Vietnam | Urban/ rural | HIV | 1108 nursing mothers | Quantitative | Assess early uptake of HIV screening and the provision of HIV counselling among pregnant women |
| Pharris [ ] | 2011 | Vietnam | Urban | HIV | 1108 pregnant women who attend antenatal care at primary and higher-level health facilities | Quantitative | Assess early uptake of HIV testing and the provision of HIV counselling among pregnant women |
| Khuu [ ] | 2018 | Vietnam | Urban | HIV | 320 women who were tested during ANC | Quantitative | Identify reasons for late HIV screening among pregnant women |
| Chu [ ] | 2019 | Vietnam | Urban/ rural | HIV | 1484 women aged 15 to 49 years having a live birth within the last 2 years | Quantitative | Assess the socioeconomic inequalities in HIV screening during ANC |
| Bharucha [ ] | 2005 | India | Urban | HIV | 6,702 pregnant women presenting in labour | Quantitative | Explore factors affecting the eligibility and acceptability of voluntary counselling and rapid HIV testing |
| Rogers [ ] | 2006 | India | Rural | HIV | 202 pregnant women attending a rural ANC clinic | Quantitative | Investigate HIV-related knowledge, attitudes toward infant feeding practices, and perceived benefits and risks of HIV screening |
| Sinha [ ] | 2008 | India | Rural | HIV | 400 women that have gave birth in the previous 12 months | Quantitative | Investigate HIV screening among rural women during pregnancy |
| Sarin [ ] | 2013 | India | Rural | HIV | 357 women who had given birth in the last two years | Quantitative | Examine the prevalence and the barriers to HIV screening among pregnant women vulnerable to HIV due to their spouses’ risky behaviours |
| Sharma [ ] | 2022 | India | Urban/ rural | HIV | 122,351 women aged 15–49 | Quantitative | Determine the factor associated with HIV screening during ANC |
| Lubis [ ] | 2019 | Indonesia | Urban/ rural | HIV | 20 private midwives | Qualitative | Examine midwives’ perceptions of barriers and enabling factors about referring pregnant women for HIV screening |
| Wulandari [ ] | 2019 | Indonesia | Urban/ rural | HIV | 619 women to voluntary HIV counselling and screening clinics | Quantitative | Examine the rates of HIV screening uptake among pregnant women attending private midwife clinics |
| Baker [ ] | 2020 | Indonesia | Rural | HIV, syphilis | 3382 pregnant women and 40 health workers involved in screening | Mixed-methods | Explore current practice, barriers and facilitators in the delivery of antenatal testing for anaemia, HIV and syphilis |
| Pakki [ ] | 2020 | Indonesia | Rural | HIV | 42 health workers managers | Quantitative | Investigate the influence of training given to health workers on HIV testing uptake by pregnant women |
| Setiyawati [ ] | 2021 | Indonesia | Urban | HIV | 350 housewives in districts that already implemented prevention mother-to-child transmission program | Quantitative | Assess the factors that influence the housewife attitude toward HIV testing |
| Kakimoto [ ] | 2007 | Cambodia | Urban | HIV | 315 mothers who came to a childhood immunization with a child aged 6–24 months | Quantitative | Assess predictive determinants for HIV testing |
| Sasaki [ ] | 2010 | Cambodia | Urban | HIV | 600 eligible mothers who were admitted to the hospital after delivery | Quantitative | Assess the prevalence of and barriers to HIV screening |
| Lee [ ] | 2005 | Hong Kong | Urban | HIV | 3,500 pregnant women attending their first ANC visit | Quantitative | Investigate acceptance of universal HIV antibody screening programme |
| Munkhuu [ ] | 2006 | Mongolia | Urban | Syphilis | 150 ANC providers and 27 senior doctors | Qualitative | Assess ANC providers’ practices and opinions toward antenatal syphilis screening |
| Todd [ ] | 2008 | Afghanistan | Urban | HIV, syphilis, hepatitis B | 114 doctors and midwives | Quantitative | Determine attitudes toward and utilization of testing for HIV, syphilis, and hepatitis B among obstetric care providers |
| Crozier [ ] | 2013 | Thailand | Urban | HIV | 38 migrant pregnant women who had been through the HIV screening process 2013and 26 health personnel | Qualitative | Explore factors that relate to HIV screening decisions for migrant women |
| Li [ ] | 2014 | China | Urban | HIV | 500 pregnant women recruited during their antenatal visit | Quantitative | Assess the prevalence of the willingness for HIV testing among pregnant women and cognitive factors associated with it |
In the four studies that used qualitative methods, pregnant women were interviewed as well as other individuals such as health providers, district managers, husbands, and mothers. Sample sizes in quantitative studies ranged from 114 to 122,351 pregnant women, most often recruited during ANC visits. The quantitative studies were all cross-sectional except one from Indonesia, which was longitudinal [ 25 ]. Most quantitative studies used logistic regression models to determine the association between potential barriers and the outcome of interest.
Overviews of the barriers and the facilitators identified
The barriers and facilitators identified in the included articles are presented based on the categories of the Andersen’s conceptual model ( Table 3 and Fig 2 ).

| Citation | Date | Country | Diseases | Predisposing characteristics | Enabling factors | Need factors |
|---|---|---|---|---|---|---|
| Bharucha [ ] | 2005 | India | HIV | Facilitators: • Being older • Living closer to the hospital | Barriers: • Being too far along in the birth delivery process when the opportunity to test arises Facilitators: • Having had antenatal care in the hospital rather than in other health facilities | |
| Dinh [ ] | 2005 | Vietnam | HIV | Barriers: • Being a housewife • Low level of education | Barriers: • Fear of husband’s disapproval • Perception of poor healthcare availability | Barriers: • Low-risk perception |
| Lee [ ] | 2005 | Hong Kong | HIV | Facilitators: • High level of education • Good HIV knowledge • Access to HIV information by means of posters, pamphlets, videos and group talks | Facilitators: • Healthcare workers’ recommendations to be screened | Barriers: • No or low-risk perception Facilitators: • Good perceived benefits of screening |
| Rogers [ ] | 2006 | India | HIV | Barriers: • Low knowledge of HIV | Barriers: • Fear of negative reactions from husbands, parents, and community • Fear of stigma and discrimination | |
| Munkhuu [ ] | 2006 | Mongolia | Syphilis | Barriers: • Low knowledge of syphilis • Being poor • Long travel distance to get tested | Barriers: • Limited time for screening due to antenatal visits starting late in pregnancy • Complexity of testing service system • Undersupplied screening materials • Healthcare workers not in favour of screening | Barriers: • Reporting previous sexually transmitted diseases |
| Kakimoto [ ] | 2007 | Cambodia | HIV | Facilitators: • Basic knowledge of HIV transmission • High partner education level | Barriers: • Need to obtain husband’s approval to be tested | |
| Sinha [ ] | 2008 | India | HIV | Barriers: • Low awareness of existing HIV testing facilities | Barriers: • Never received HIV counselling before | |
| Todd [ ] | 2008 | Afghanistan | HIV, syphilis, hepatitis B | Facilitators: • High acceptance of screening by providers Barriers: • Providers’ perceptions that infections were rare • Provider’s low perceived likelihood of infection based on healthy appearance • Stigma toward infected individuals • Need to obtain husband’s approval to be tested | ||
| Nguyen [ ] | 2010 | Vietnam | HIV | Barriers: • High distance to the hospital | ||
| Sasaki [ ] | 2010 | Cambodia | HIV | Barriers: • Low knowledge of HIV | Barriers: • Lack of access to antenatal care services • Need to obtain husband’s approval to be tested | |
| Hạnh [ ] | 2011 | Vietnam | HIV | Facilitators: • First antenatal check-up at primary health facilities rather than at district and provincial health facilities | ||
| Pharris [ ] | 2011 | Vietnam | HIV | Facilitators: • Younger age • Residence in a semi-urban area • Higher economic status | Barriers: • Low perception of risk | |
| Crozier [ ] | 2013 | Thailand | HIV | Barriers: • Low knowledge of HIV and mother-to-child transmission | Barriers: • Language differences between health worker and pregnant women • Concern about the reactions of health workers • Financial barriers • Costs and time of transportation • Provider’s lack of time to inform women properly • Having only one antenatal check-up • Lack of support from husband | Barriers: • Low perception of risk |
| Sarin [ ] | 2013 | India | HIV | Facilitators: • More than six years of education • Good knowledge of HIV | Facilitators: • Discussions with husband about HIV • Seeking antenatal care in government district hospitals and private clinics as opposed to community health centres (not equipped with either HIV counselling or testing facilities) | |
| Li [ ] | 2014 | China | HIV | Facilitators: • Good knowledge of HIV | Facilitators: • Less perception of social stigma | Facilitators: • High perception of risk |
| Khuu [ ] | 2018 | Vietnam | HIV | Barriers: • Younger than 30 years old • Nine or fewer years of education • Working as a homemaker or worker/farmer • Living 20km or more from the hospital | Barriers: • Having received antenatal care at private clinic/hospital only | Barriers: • Low perceived benefits of screening |
| Chu [ ] | 2019 | Vietnam | HIV | Barriers: • Belonging to ethnic minorities • Having primary or less education • Being poor • Living in rural areas | ||
| Lubis [ ] | 2019 | Indonesia | HIV | Facilitators: • Free HIV screening • Reward and punishment system to motivate providers • Training for health workers Barriers: • Fear of stigma • Limited voluntary counselling and testing opening hours do not cater for those in employment • Not a one-roof for ANC and VCT services • Providers disguising or not revealing purpose of the blood testing for fear of causing offense | ||
| Wulandari [ ] | 2019 | Indonesia | HIV | Facilitators: • Living in urban area | ||
| Baker [ ] | 2020 | Indonesia | HIV, syphilis | Barriers: • National policy on testing not widely disseminated • Testing not seen as a priority intervention • Multiple small-scale funding sources • Tests seen as expensive by pregnant women • Lack of knowledge and training of providers • Shortage of laboratory personnel • Shortage of tests and laboratory resources • Stigma amongst providers and community • Lack of time from pregnant women • Fear of the results | Barriers: • Perceived low prevalence | |
| Pakki [ ] | 2020 | Indonesia | HIV | Facilitators: • Health workers training on predisposing factors of provider-initiated testing and counselling of HIV | ||
| Setiyawati [ ] | 2021 | Indonesia | HIV | Barriers: • Pregnant women’s beliefs that their husbands have a bad attitude towards HIV testing | Barriers: • Low perceived benefits of screening | |
| Sharma [ ] | 2022 | India | HIV | Barriers: • Low educational level • Low knowledge of HIV • Being poor • Living in rural area • Low exposure to mass media |
Predisposing characteristics
Several predisposing characteristics were reported as either barriers or facilitators to antenatal screening for HIV and syphilis. In three studies conducted in Vietnam and India, age was associated with antenatal screening of HIV [ 22 , 32 , 33 ]. Pharris et al. [ 32 ] found that younger Vietnamese women were more likely to be screened while Bharucha et al. [ 33 ] found the opposite result in India. Khuu et al. [ 22 ] identified being younger than 30 years old as a barrier to antenatal screening.
Low education status of pregnant women was a barrier to antenatal screening in three studies conducted in Vietnam [ 22 , 23 , 29 ] and one in India [ 28 ]. Similarly, one study conducted in Hong Kong [ 39 ] and one in India [ 36 ] identified higher education as a facilitator to antenatal screening. However, the level of education associated with a positive likelihood of being screened varied between studies. For example, Khuu et al. [ 22 ] showed that nine or more years of education was associated with more acceptance of screening in Vietnam, whereas Sarin et al. [ 36 ] showed that this was true at more than six years of education in rural India.
Pregnant women’s knowledge about HIV and PMTCT was associated with antenatal screening decisions. Lack of knowledge about HIV amongst pregnant women [ 28 , 34 , 36 , 38 ], about the MTCT services [ 34 ], and about the availability of HIV testing facilities [ 35 ] were identified as barriers to screening in four studies in India, one in Cambodia and one in Thailand. Similarly, three studies conducted in Cambodia, Hong Kong and China found that a better knowledge of HIV amongst pregnant women was associated with a higher screening uptake [ 37 , 39 , 41 ]. Moreover, Munkhuu et al. [ 19 ] found similar results for syphilis in their study conducted in Mongolia. Lack of knowledge about syphilis amongst pregnant women was associated with lower screening uptake. A study conducted in India [ 28 ] found that low exposure to mass media was associated with lower HIV screening uptake. Similarly in Hong Kong, Lee et al. [ 39 ] identified access to HIV information by means of posters, pamphlets, videos, and group talks as a facilitator to screening.
Enabling factors
The role of enabling factors such as wealth, place of residence, husbands and health workers’ roles, social and cultural norms or screening cost has been discussed in several articles.
Low household wealth or socio-economic status was a barrier even in countries where antenatal screening was free of charge. Three studies conducted in Mongolia, Vietnam, and India found low socio-economic status as being a barrier to antenatal screening for HIV [ 19 , 23 , 28 ]. Pharris et al. [ 32 ] identified higher economic status as a facilitator to antenatal screening for HIV in Vietnam.
Various studies have shown that the place of residence was associated with antenatal screening for HIV [ 22 , 23 , 25 , 28 , 30 , 32 , 33 ] and syphilis [ 19 ]. A study conducted in Vietnam [ 23 ] and another conducted in India [ 28 ] identified living in a rural area as a barrier to antenatal screening for HIV. Similarly, Wulandari et al. [ 25 ] and Pharris et al. [ 32 ] found that living in an urban area and a semi-urban area were facilitators to antenatal screening of HIV in Vietnam and Indonesia respectively. Proximity to the hospital is also a factor influencing antenatal screening uptake. Khuu et al. [ 22 ] and Nguyen, Christoffersen, and Rasch [ 30 ] found that living further away from the hospital (over 20km in the case of Khuu et al.) was a barrier to antenatal screening for HIV. Similar results were found by Munkhuu et al. [ 19 ] in Mongolia for the antenatal screening of syphilis. Meanwhile, Bharucha et al. [ 33 ] identified living closer to the hospital as a facilitator for antenatal screening of HIV in India.
Two studies conducted in Vietnam found a significant effect of occupation on the decision to be tested. For example, housewives, or labourers/farmers were less likely to be tested for HIV [ 22 , 29 ]. Kakimoto et al. [ 37 ] identified high partner education level as a facilitator to antenatal screening in Cambodia. Meanwhile, Chu, Vo [ 23 ] found a negative association between belonging to ethnic minorities and being tested during pregnancy.
Several articles identified that their husband play a key role in women’s decision to be screened. Fear of negative reactions from their husbands [ 34 ], husband’s disapproval [ 29 ] and lack of support [ 40 ], and beliefs that their husbands have a bad attitude towards HIV testing [ 27 ] were identified as barriers to screening in India, Thailand, Indonesia and Vietnam respectively. Two studies conducted in Cambodia [ 37 , 38 ] found that the perceived need to obtain partner’s authorisation is a barrier to screening for HIV. Similar findings were found in Afghanistan by Todd et al. [ 21 ] for antenatal screening of syphilis and hepatitis B. Similarly, Sarin et al. [ 36 ] reported that having discussions with spouses about HIV in India encouraged women’s screening for HIV.
Various studies have shown that social and cultural factors were key barriers to antenatal screening for HIV, syphilis or hepatitis B. Todd et al. [ 21 ] identified stigma toward infected people as a barrier to antenatal screening for HIV, syphilis, and hepatitis B in Afghanistan. Similar results were found by Baker et al. [ 20 ] in Indonesia for the screening of HIV and syphilis, and Lubis et al. [ 24 ] and Rogers et al. [ 34 ] for the screening of HIV. This last article also identified the fear of negative reactions from parents and community as a barrier. Similarly, Li et al. [ 41 ] found that lower perception of social stigma was associated with higher screening uptake.
Time was also associated with antenatal screening decisions for HIV and syphilis. It was a barrier both from the supply and the demand side. Working pregnant women reported that limited opening hours of screening centres were a major health-facility related barrier to antenatal screening for HIV in Indonesia [ 24 ]. Limited time to inform women properly about HIV during pregnancy and antenatal screening [ 40 ] as well as limited time to perform screening for syphilis [ 19 ] were barriers to antenatal screening in Thailand and Mongolia. From the demand side, long travel time to access antenatal screening services was associated with lower HIV screening uptake in Thailand [ 40 ]. Similarly, lack of time was identified as a barrier to screening for HIV and syphilis in Indonesia by Baker et al. [ 20 ]. Meanwhile, Bharucha et al. [ 33 ] found that being offered testing too late in pregnancy as associated with lower screening uptake for HIV.
The type of screening provider was a factor associated with screening in various studies. Hạnh, Gammeltoft, and Rasch [ 31 ] showed that, in Vietnam, having the first antenatal check-up at a commune health station was a factor associated with an increased probability of being tested, compared with district and provincial health facilities. Similarly and in the same country, having received ANC only at a private clinic/hospital was found to be a barrier [ 22 ]. However, in India, Sarin et al. [ 36 ] found that seeking ANC at government district hospitals and private clinics, as opposed to community health centres not equipped with either HIV counselling or testing facilities, had a positive effect on the probability of receiving HIV screening. Similar results were found by Bharuch et al. [ 33 ] in India. Some facilities lack screening materials and this was associated with lower screening of syphilis in Mongolia [ 19 ] and lower screening of HIV and syphilis in Indonesia [ 20 ]. In addition, a study carried out in Indonesia [ 24 ] revealed that the lack of antenatal care and screening services in the same building was a barrier to HIV screening. In Cambodia, the lack of access to ANC services outside the capital city was a barrier to screening for HIV [ 38 ].
Healthcare workers play a key role in screening decisions. In Vietnam, Dinh, Detels and Nguyen [ 29 ] found that a poor perception of healthcare availability was negatively associated with screening for HIV. Fear that healthcare workers would become impatient with them or that their questions would not be considered important was a barrier in Thailand [ 40 ], and concern that healthcare workers were opposed to antenatal screening for syphilis impeded testing in Mongolia [ 19 ]. Similarly, Lee et al. [ 39 ] identified health worker recommending HIV testing as a facilitator of screening. A study conducted in Vietnam [ 32 ] identified never having received antenatal HIV counselling as a barrier to screening and another identified a language barrier between health workers and women as barriers [ 40 ]. High acceptance of screening for HIV, syphilis and hepatitis B was also a factor increasing screening uptake in Afghanistan [ 21 ]. Pakki et al. [ 26 ] and Lubis et al. [ 24 ] found that, in Indonesia, health worker training as well as reward and punishment system to motivate them was associated with higher antenatal HIV screening. This is consistent with findings reported in Indonesia for HIV and syphilis screening [ 20 ]. Todd et al. [ 21 ] found that provider perceptions of low infection rates and assumptions on a person’s likelihood of infection based on a healthy appearance were associated with lower screening uptake of HIV, syphilis and hepatitis B in Afghanistan. Baker et al. [ 20 ] also identified shortage of laboratory personnel as a barrier to screening.
Costs of screening was also identified as factor influencing HIV and syphilis screening uptake. Tests being seen as expensive by pregnant women was identified as a barrier to HIV and syphilis screening in Indonesia [ 20 ]. Similarly, Crozier et al. [ 40 ] found that costs of screening and transportation represent barriers to screening of HIV and syphilis in Thailand.
At the national-level, enabling factors were identified by two studies in Mongolia and Indonesia [ 19 , 20 ]. Munkhuu et al. [ 19 ] identified the complexity of the syphilis testing service system as a barrier to antenatal screening. Similarly, Baker et al. [ 20 ] found that poor dissemination of national policy on screening, not seeing screening as a priority intervention, and funding consisting of multiple small-scale sources were barriers to HIV and syphilis screening in Indonesia.
Finally, Crozier, Chotiga et Pfeil [ 40 ] showed that having only one ANC check-up was associated with low screening uptake.
Need factors
Few need factors were identified as barriers or facilitators in antenatal screening for HIV and syphilis. Four studies conducted in Hong Kong, Vietnam and Thailand found that low perceived risk of HIV was associated with low screening [ 29 , 32 , 39 , 40 ]. Similarly, Lee, Yang, and Kong [ 41 ] found that, in China, high perceived risk of HIV was associated with high screening. In a study investigating barriers and facilitators in the delivery of antenatal testing for anaemia, HIV, and syphilis, Baker et al. [ 20 ] identified perceived low prevalence of HIV and syphilis as barriers to antenatal screening in Indonesia. Two studies found that believing that HIV testing was not important during pregnancy was associated with a lower screening uptake in Indonesia and Vietnam [ 22 , 27 ]. Similar Lee et al. [ 39 ] identified the perception of the benefits of HIV screening as a factor facilitating it. Finally, Munkhuu et al. [ 19 ] found that women who previously reported STIs were less likely to be screened in Mongolia.
This study is the first to provide a narrative synthesis of the current literature on barriers and facilitators to antenatal screening for HIV, syphilis and hepatitis B in Asia. This systematic review of qualitative, quantitative and mixed-method studies shows that there are research gaps into the factors influencing screening for syphilis and hepatitis B, with most of the studies reviewed focusing on HIV. This review therefore effectively allows conclusions to be drawn about HIV alone.
Antenatal screening for HIV in Asia is influenced by a range of factors including predisposing characteristics (age, education level, wealth, place of residence, knowledge about HIV), enabling factors (husband support, health facilities characteristics, health workers’ support and training) and need factors (risk perception, perceived benefits of screening). These factors are similar to those identified in a review conducted by Blackstone et al. [ 12 ] in sub-Saharan Africa. In our literature review, as in the sub-Saharan African context, being better-off and highly educated were identified as facilitators. In both contexts, pregnant women’s lack of knowledge about HIV appears to be a significant barrier to antenatal HIV screening. Our results suggest that antenatal screening could be improved by facilitating access to information for women, their husbands and health workers. Most studies have emphasised the importance of improving dissemination of information about HIV and HIV testing in order to improve uptake of antenatal screening. Unlike Blackstone et al.’s review of the literature in the sub-Saharan African context [ 12 ], our review did not identify fear of results as such as a barrier to testing, but more broadly fear of partner reactions and potential violence in the event of a positive result. We did not find that cultural gender norms to be barrier, such as "testing is a woman’s business", as found by Blackstone et al. [ 12 ]. However, women in this review mentioned the need to obtain a husband’s approval to undergo screening. In both African and Asian contexts, societal stigma towards HIV-positive people proved to be a major barrier to HIV testing. Our findings, and those of Blackstone et al. [ 12 ], suggest that antenatal screening could be improved by strengthening the health care system. Both reviews highlighted the role of healthcare and communication professionals in increasing antenatal screening rates. In the sub-Saharan African context the perception of screening being mandatory was a barrier to screening, but this did not emerge in our literature review.
Although the studies we reviewed were all conducted in Asia, they spanned very different contexts. It is reasonable to assume that the barriers to antenatal screening will differ between Hong Kong and India for instance. Guidelines about screening and adherence to guidelines differ between countries. A review of maternal health care policies in eight countries in the Western Pacific region [ 42 ] found that WHO recommendations on antenatal HIV screening were not included in antenatal care guidelines in two countries. In 2018, 37 countries in the Asia Pacific region promoted antiretroviral therapy for all pregnant and breastfeeding women living with HIV, but in six of these countries, the policy is being implemented in less than 50% of all maternal and child health sites [ 43 ]. Reported barriers in the Hong Kong study were mainly focused on the demand side [ 39 ], whereas the Mongolia study identified many supply-side barriers [ 19 ]. This highlights the need for qualitative studies in Asian contexts to investigate context-dependent factors that may be missed in quantitative studies.
As stigmatisation of people with STDs is one of the main factors preventing pregnant women from being screened, interventions should provide information and counselling to pregnant women and their husbands, tailored to low-literacy populations to help reduce stigma and increase uptake [ 36 , 38 , 39 ]. Raising awareness within communities of the importance of male partner involvement, the benefits of screening and adherence to treatment could increase demand for antenatal screening services. However, studies on awareness campaigns about HIV in Vietnam [ 44 ] and Thailand [ 45 ] showed that the stigma attached to social judgement is difficult to reduce. Various studies recommended the integration of HIV screening into community level ANC services [ 23 , 25 , 30 , 31 , 39 ] and the development of opt-out approaches for those who prefer not to test [ 29 , 35 ], as recommended in sub-Saharan Africa by Blackstone et al. [ 12 ]. We found that husbands play a key role in encouraging pregnant women to undergo screening. Interventions to improve husbands’ knowledge and involvement in maternal and newborn health had a positive impact on maternal health behaviour in Bangladesh [ 46 ] and Nepal [ 47 ]. To reduce social and financial barriers to antenatal screening, screening should be offered to pregnant women universally free of cost [ 32 , 39 ]. Currently, national budgets do not cover all the costs associated with antenatal screening in all Asian countries. In the 17 Asian countries for which data on the cost of screening pregnant women for HIV, syphilis and hepatitis B were available in 2017, HIV screening of pregnant women was free in all of these countries, syphilis screening in 14 countries and hepatitis B screening was free in eight countries [ 11 ]. Finally, the quality of services depends on the availability and capacity of healthcare workers. To reduce the persistence of inappropriate healthcare practices in pregnancy, interventions need to develop health worker training programmes on STIs and pregnancy screening. A successful initiative in Cambodia in decreasing risky sexual intercourse and improving the access to sexual and reproductive health care services has focused on training community health workers in sexual and reproductive, maternal, neonatal, child and adolescent health [ 48 ].
Adolescent pregnancy is still common in the region with 3.7 million births to adolescent girls aged 15–19 every year in Asia and the Pacific [ 49 ]. Pregnant adolescents are very vulnerable and are known to have poor outcomes for both mother and child [ 50 ]. This systematic review of the literature highlighted a lack of age-specific data, particularly in relation to adolescent pregnancy, and confirmed the need to fill this research gap. Similarly, a systematic literature review of interventions addressing health outcomes for pregnant adolescents in low- and middle-income countries highlighted the need to develop studies to design high-quality care and services for pregnant adolescents [ 51 ].
Several limitations to this study should be noted. Firstly, most studies sampled pregnant women through ANC services. However, women who have not sought ANC may face the greatest barriers to testing. Due to resource constraints, only articles in English were reviewed, which may limit access to the grey literature and studies published in other languages (especially Chinese). Finally, different studies were undertaken in different contexts and using different methods. This heterogeneity limits our ability to compare between studies. However, this systematic review follows a rigorous method of article selection and analysis. It complements existing literature reviews on barriers to antenatal screening, particularly in sub-Saharan Africa [ 12 , 52 ].
The main barriers to antenatal screening in this systematic review were stigmatisation of infected individuals, lack of involvement of husbands and healthcare system factors. To improve uptake of antenatal screening interventions to improve community and husband involvement, awareness campaigns with communities and health workers, and training of health workers on STI issues are needed. While countries vary in their contexts and implementation of international recommendations on integrated antenatal screening for STIs, in all settings the planning, implementation, reporting and monitoring of interventions to eliminate mother-to-child transmission require coordination between different health system stakeholders at national, regional and local levels to avoid gaps or duplication. Global, regional and national guidelines need to be harmonised to avoid gaps and duplication between disease-specific and maternal and child health programs and guidelines. Integration of services for different diseases should be prioritised where possible. However, studies to examine the barriers and facilitators to antenatal screening for syphilis and hepatitis B and to examine the behavioural determinants of antenatal screening in Asia are still needed.
Supporting information
Funding statement.
The authors received no specific funding for this work.
Data Availability
- PLoS One. 2024; 19(5): e0300581.
Decision Letter 0
19 May 2023
PONE-D-23-03027Barriers and facilitators to antenatal screening for sexually transmitted diseases in Asia: a scoping review.PLOS ONE
Dear Dr. Sabin,
Thank you for submitting your manuscript to PLOS ONE. After careful consideration, we feel that it has merit but does not fully meet PLOS ONE’s publication criteria as it currently stands. Therefore, we invite you to submit a revised version of the manuscript that addresses the points raised during the review process.
==============================
Carefully consider both reviewers' comments especially with regards to the framework that was used for the study and also labelling of the study as a scoping review. The various components and processes that are necessary for a scoping review ought to be presented in the manuscript.
Please submit your revised manuscript by Jul 03 2023 11:59PM. If you will need more time than this to complete your revisions, please reply to this message or contact the journal office at gro.solp@enosolp . When you're ready to submit your revision, log on to https://www.editorialmanager.com/pone/ and select the 'Submissions Needing Revision' folder to locate your manuscript file.
Please include the following items when submitting your revised manuscript:
- A rebuttal letter that responds to each point raised by the academic editor and reviewer(s). You should upload this letter as a separate file labeled 'Response to Reviewers'.
- A marked-up copy of your manuscript that highlights changes made to the original version. You should upload this as a separate file labeled 'Revised Manuscript with Track Changes'.
- An unmarked version of your revised paper without tracked changes. You should upload this as a separate file labeled 'Manuscript'.
If you would like to make changes to your financial disclosure, please include your updated statement in your cover letter. Guidelines for resubmitting your figure files are available below the reviewer comments at the end of this letter.
If applicable, we recommend that you deposit your laboratory protocols in protocols.io to enhance the reproducibility of your results. Protocols.io assigns your protocol its own identifier (DOI) so that it can be cited independently in the future. For instructions see: https://journals.plos.org/plosone/s/submission-guidelines#loc-laboratory-protocols . Additionally, PLOS ONE offers an option for publishing peer-reviewed Lab Protocol articles, which describe protocols hosted on protocols.io. Read more information on sharing protocols at https://plos.org/protocols?utm_medium=editorial-email&utm_source=authorletters&utm_campaign=protocols .
We look forward to receiving your revised manuscript.
Kind regards,
Gifty Dufie Ampofo, M.D., Ph.D
Academic Editor
Journal requirements:
When submitting your revision, we need you to address these additional requirements.
1. Please ensure that your manuscript meets PLOS ONE's style requirements, including those for file naming. The PLOS ONE style templates can be found at
https://journals.plos.org/plosone/s/file?id=wjVg/PLOSOne_formatting_sample_main_body.pdf and
https://journals.plos.org/plosone/s/file?id=ba62/PLOSOne_formatting_sample_title_authors_affiliations.pdf .
2. Please include a copy of Table 4 and 5 which you refer to in your text on page 6.
3. Please include captions for your Supporting Information files at the end of your manuscript, and update any in-text citations to match accordingly. Please see our Supporting Information guidelines for more information: http://journals.plos.org/plosone/s/supporting-information .
[Note: HTML markup is below. Please do not edit.]
Reviewers' comments:
Reviewer's Responses to Questions
Comments to the Author
1. Is the manuscript technically sound, and do the data support the conclusions?
The manuscript must describe a technically sound piece of scientific research with data that supports the conclusions. Experiments must have been conducted rigorously, with appropriate controls, replication, and sample sizes. The conclusions must be drawn appropriately based on the data presented.
Reviewer #1: No
Reviewer #2: No
2. Has the statistical analysis been performed appropriately and rigorously?
Reviewer #1: N/A
Reviewer #2: N/A
3. Have the authors made all data underlying the findings in their manuscript fully available?
The PLOS Data policy requires authors to make all data underlying the findings described in their manuscript fully available without restriction, with rare exception (please refer to the Data Availability Statement in the manuscript PDF file). The data should be provided as part of the manuscript or its supporting information, or deposited to a public repository. For example, in addition to summary statistics, the data points behind means, medians and variance measures should be available. If there are restrictions on publicly sharing data—e.g. participant privacy or use of data from a third party—those must be specified.
Reviewer #1: Yes
Reviewer #2: Yes
4. Is the manuscript presented in an intelligible fashion and written in standard English?
PLOS ONE does not copyedit accepted manuscripts, so the language in submitted articles must be clear, correct, and unambiguous. Any typographical or grammatical errors should be corrected at revision, so please note any specific errors here.
5. Review Comments to the Author
Please use the space provided to explain your answers to the questions above. You may also include additional comments for the author, including concerns about dual publication, research ethics, or publication ethics. (Please upload your review as an attachment if it exceeds 20,000 characters)
Reviewer #1: The topic is of great interest, however the manuscript seems hurriedly put together. Concepts involved such as Andersen's model are not clearly and coherently applied in the course of the write-up.
The title for example does not capture the full essence of the review - it seems to be based on the "regional framework for the triple elimination of MTCT of HIV, Hep B and syphillis in Asia and Pacific" (lines 99 - 101)- that should have reflected clearly in the title. Such an understanding should have been provided briefly in the "Background" section of the script.
Secondly, the target population of the review was not clear right from the "title". Who did the review focus on - pregnant women, healthcare providers, relatives, etc. or all of them? That is not clear from the manuscript.
The objectives of the review as stated in lines 74 and 75 are not meant for a scoping review, but some other approaches that would generate clear evidence such as a review of qualitative evidence.
The methods section has lots of lapses.
a. A key concept such as the "population of the review" is not defined. The "search strategy" should have been systematically presented - e.g., keywords/ subject headings/ index terms that were used, example of a search strategy of at least one of the databases should have been placed in the appendices; the search should have been as exhaustive as possible - searching two databases does not sound exhaustive enough.
b. The "inclusion and exclusion criteria" should have been clearly defined each criterion - this subsection at best is confusing to the reader as it does not serve its purpose of clearly pointing out how studies were included in the review. Studies of experimental designs were excluded with no apparent reasons as to why they were.
c. Under "Data extraction", the Andersen's framework was said to have been the guide - it would have been great to have this clearly "tabulated" with "findings" related to each component of the framework duely and systematically presented. The quality of studies was assessed, but this outcome did not feature further into any decision-making or discussion as to how study quality influenced the review process.
d. Andersen's model as defined in lines 123 - 124 does not seem to be in sync with the cited publication (11), i.e., predisposing, enabling, and needs factors. "Enabling factors" were not given the prominence required.
Aside the mention of "facilitators" on line 147, this key component of the review was hardly addressed. Furthermore in the results section, the nature of the findings as were presented did not necessarily aptly fit the defined factors under the Andersen model.
In its current form, this manuscript in my view is not fit for publication.
Reviewer #2: Review Comments on manuscript PONE-D-23-03027
…..perhaps the title should be restricted to HIV, Syphilis and Hepatitis B rather than ‘sexually transmitted diseases’
Despite being a scoping review, a little more detail will improve the Background and situate arguments in better context.
• Lines 50/51…….the authors can provide recent data on the morbidity and mortality they refer to…..first globally and in the Asian context
Quantify the prevalence of these STDs in Asia (at least present data from some Asian countries)
• Lines 58/61…..can the authors assign, at least, an estimate of how many children are born to these STDs? Can they quantify antenatal screening for STDs in Asia? Can they give us an idea of how low is ‘low’.
I think it would be useful to give a brief overview of this WHO regional framework and what different prescriptions it gave compared to whatever existed before its formation
• Lines 68/70……The authors may want to give more meaning to the listed ‘barriers’ and how they relate to uptake of HIV screening services.
It would be particularly interesting to see what the story is for “health system and health care provider issues”
In many jurisdictions in sub-Saharan Africa, HIV screening is part of the antenatal care package and is offered using the opt-out model.
• There is no literature review summarising the research-based evidence on barriers and facilitators to antenatal screening for STDs in the Asian context.
Why is the statement above a problem? What is the burden of maternal and child morbidity and mortality in Asia in the context of HIV, Syphilis, Hepatitis C? What are the fall-outs from the supposed low uptake of available screening services? What do we stand to lose if this review is not done to better understand barriers and facilitators that can help inform useful interventions?
• Can the authors rewrite the Methods section without ‘We’?
• Line 84. We used a very inclusive search strategy to ensure that no item was missed…..Can you give a 100% guarantee no item was missed?
• There appears to be something in Line 92 that is not supposed to be there
Inclusion and Exclusion Criteria
The inclusion and exclusion criteria appear to be ‘all over the place’. They can be made more focused.
We did not include studies investigating antenatal screening for other STDs……..This does not qualify as an exclusion criterion because you have earlier specified that you are dealing with HIV, Hep B and Syphilis
• The data extraction sub-section has nothing on “facilitators”
• Line 121…..the authors may want to justify the choice of Andersen’s conceptual model over other models they could have used.
• For Table 1, I think the year the study was conducted ought to be in separate column by itself. This will enable readers to relate them to implementation of the MDGs and contextualize them.
• I have some questions relating to Fig.1;
……you mentioned Google Scholar but I don’t see in the flow diagram
…….I am struggling to understand how you excluded 546 articles because the studies were not conducted in Asia when ‘Asia’ should have been a key part of your search strategy. Kindly elaborate on how this happened.
• Lines 210/211…….please give more meaning to ‘perceptions of poor healthcare support’ and ‘concerns about the reactions of healthcare workers
Secondly, of the 16 articles, 15 were on HIV and 1 was on Syphilis with nothing on Hepatitis B. In this context, I fail to see how you can make any reasonable pronouncements on Syphilis and Hepatitis B screening uptake.
On this basis, I suggest you drop off Syphilis and Hep B and make your work entirely about uptake of HIV screening than about STDs and appropriately reorient your discussion to that effect.
I look forward to reading a new version of your work.
6. PLOS authors have the option to publish the peer review history of their article ( what does this mean? ). If published, this will include your full peer review and any attached files.
If you choose “no”, your identity will remain anonymous but your review may still be made public.
Do you want your identity to be public for this peer review? For information about this choice, including consent withdrawal, please see our Privacy Policy .
Reviewer #1: Yes: Yeetey ENUAMEH
[NOTE: If reviewer comments were submitted as an attachment file, they will be attached to this email and accessible via the submission site. Please log into your account, locate the manuscript record, and check for the action link "View Attachments". If this link does not appear, there are no attachment files.]
While revising your submission, please upload your figure files to the Preflight Analysis and Conversion Engine (PACE) digital diagnostic tool, https://pacev2.apexcovantage.com/ . PACE helps ensure that figures meet PLOS requirements. To use PACE, you must first register as a user. Registration is free. Then, login and navigate to the UPLOAD tab, where you will find detailed instructions on how to use the tool. If you encounter any issues or have any questions when using PACE, please email PLOS at gro.solp@serugif . Please note that Supporting Information files do not need this step.
Author response to Decision Letter 0
Dear Doctor Ampofo,
We thank you and the reviewer for your time and generous comments provided on our manuscript PLONE-D-23-03027 entitled "Barriers and facilitators to antenatal screening for sexually transmitted diseases in Asia: a scoping review", and we thank you for the opportunity to address these comments. After consideration of your comments, we have made several improvements.
The comments provided are shown in bold below, with our responses in italics.
Editor's Comments to the Author:
1. Please ensure that your manuscript meets PLOS ONE's style requirements, including those for file naming.
Response: We have ensured that the manuscript meets the stylistic requirements of PLOS ONE.
2. Please include a copy of Tables 4 and 5 which you refer to in your text on page 6.
Response: A copy of tables 4 and 5 has been included under the name S2 Table and S3 Table.
3. Please include captions for your Supporting Information files at the end of your manuscript, and update any in-text citations to match accordingly.
Response: Captions for our Supporting Information files have been included at the end of the manuscript.
Reviewers’ Comments to the Author:
Reviewer #1:
The topic is of great interest, however the manuscript seems hurriedly put together. Concepts involved such as Andersen's model are not clearly and coherently applied in the course of the write-up.
Response: Thank you for your comment. We now define Andersen’s model (lines 148-153) and clearly and systematically apply the concepts cited. We have added Table 3 and systematically structured our results according to each component of Andersen’s model. The "facilitators" have been taken into account appropriately in the review.
The title for example does not capture the full essence of the review - it seems to be based on the "regional framework for the triple elimination of MTCT of HIV, Hep B and syphilis in Asia and Pacific" (lines 99 - 101)- that should have reflected clearly in the title. Such an understanding should have been provided briefly in the "Background" section of the script.
Response: We have changed the initial title from “Barriers and facilitators to antenatal screening for sexually transmitted diseases in Asia: a scoping review” to “A systematic review of barriers and facilitators to antenatal screening for HIV, syphilis or hepatitis B in Asia: perspectives of pregnant women, their relatives and health care providers.” The role of the WHO framework as the basis for this study has also been clarified in the background section (lines 76-89).
Response: On the basis of all the reviewers' comments, we decided to carry out a systematic analysis of the literature rather than a scoping review, using a second person to screen and review articles in duplicate and by searching other databases. We adapted the objectives to those of a systematic literature review (lines 113-115).
a. A key concept such as the "population of the review" is not defined. The "search strategy" should have been systematically presented - e.g., keywords/ subject headings/ index terms that were used, an example of a search strategy of at least one of the databases should have been placed in the appendices; the search should have been as exhaustive as possible - searching two databases does not sound exhaustive enough.
Response: Thank you for this comment. To make the search as exhaustive as possible and in line with other reviews of this nature, we searched Ovid (MEDLINE, Embase, PsycINFO), Scopus, Global Index Medicus and Web of Science. Our database search strategy has been included in S1 File.
Response: The eligibility criteria for the inclusion of studies have been rewritten and tabulated in Table 2 using the acronym SPlDER: S sample; P phenomenon of interest; D design; E evaluation; R research type. Our original inclusion/exclusion criteria were unchanged except that we also decided to include experimental design studies.
c. Under "Data extraction", the Andersen's framework was said to have been the guide - it would have been great to have this clearly "tabulated" with "findings" related to each component of the framework duly and systematically presented. The quality of studies was assessed, but this outcome did not feature further into any decision-making or discussion as to how study quality influenced the review process.
Response: We agree that a more systematic application of Andersen’s framework improves the paper so have rewritten the results section to clearly reflect each of the elements of the Andersen framework and added Table 3. As the aim of the review was to describe and synthesise a body of literature and not to determine effect size, we did not exclude studies on the basis of their quality assessment (lines 160-161) but we have summarised the quality assessment in S2 and S3 Tables to enable readers to see the quality of the evidence included in the review.
Response: We agree with this comment and have now given more explanation of the ‘enabling factors’ of antenatal screening (lines 151-152).
Response: As explained above we have now explicitly defined the "facilitators" in Table 1 and entirely rewritten the results section to follow the factors defined in Andersen’s model.
Response: Thank you for your detailed comments. We hope that the changes you have made will enable the study to be published.
Reviewer #2:
Title…..perhaps the title should be restricted to HIV, Syphilis and Hepatitis B rather than ‘sexually transmitted diseases’.
Response: Thank you. We have changed the title to “A systematic review of barriers and facilitators to antenatal screening for HIV, syphilis or hepatitis B in Asia: perspectives of pregnant women, their relatives and health care providers.”
Introduction: Despite being a scoping review, a little more detail will improve the Background and situate arguments in better context.
Response: We have expanded the introduction to better place the study in context. We have also changed from a scoping to a systematic review.
Lines 50/51…….the authors can provide recent data on the morbidity and mortality they refer to…..first globally and in the Asian context Quantify the prevalence of these STDs in Asia (at least present data from some Asian countries).
Response: Data on mother-to-child transmission of HIV, syphilis and hepatitis B were added to the introduction. The prevalence of the STDs considered was quantified in the introduction section.
Lines 58/61…..can the authors assign, at least, an estimate of how many children are born to these STDs? Can they quantify antenatal screening for STDs in Asia? Can they give us an idea of how low is ‘low’.
Response: We have added an estimate of the number of children born with these STDs (lines 54-59), as well as a quantification of antenatal screening for STDs in Asia (lines 63-68).
Response: Thank you for this suggestion. We have added an overview of the WHO regional framework and its main prescriptions (lines 76-87).
Lines 68/70……The authors may want to give more meaning to the listed ‘barriers’ and how they relate to uptake of HIV screening services. It would be particularly interesting to see what the story is for “health system and health care provider issues”. In many jurisdictions in sub-Saharan Africa, HIV screening is part of the antenatal care package and is offered using the opt-out model.
Response: Thank you for this suggestion. The obstacles listed have been detailed for greater clarity.
There is no literature review summarising the research-based evidence on barriers and facilitators to antenatal screening for STDs in the Asian context. Why is the statement above a problem? What is the burden of maternal and child morbidity and mortality in Asia in the context of HIV, Syphilis, Hepatitis C? What are the fall-outs from the supposed low uptake of available screening services? What do we stand to lose if this review is not done to better understand barriers and facilitators that can help inform useful interventions?
Response: We have clarified and expanded the introduction by highlighting the importance of this review (lines 88-92) and giving the reasons why a literature review in Asia is needed (lines 102-112). We now detail, in the introduction, the burden of maternal and infant morbidity and mortality in Asia within the limits of available data. We have also explained the consequences of the low uptake of screening services (lines 70-75).
Can the authors rewrite the Methods section without ‘We’?
Response: We decided to keep this section written in active voice as it is easier to understand and saves words. It is nowadays recommended for scientific writing in biomedical journals.
Line 84. We used a very inclusive search strategy to ensure that no item was missed…..Can you give a 100% guarantee no item was missed?
Response: We removed this sentence from the manuscript.
There appears to be something in Line 92 that is not supposed to be there.
Response: We removed this from the manuscript.
Inclusion and Exclusion Criteria: The inclusion and exclusion criteria appear to be ‘all over the place’. They can be made more focused. We did not include studies investigating antenatal screening for other STDs……..This does not qualify as an exclusion criterion because you have earlier specified that you are dealing with HIV, Hep B and Syphilis.
Response: We agree and have rewritten the eligibility criteria for study inclusion using the acronym SPlDER: S sample; P phenomenon of interest; D design; E evaluation; R research type.
The data extraction sub-section has nothing on “facilitators”
Response: In the methods, we have added a subsection on the extraction of data and explained how we focus upon both barriers and facilitators to antenatal screening within the structure of Andersen’s framework (Table 3).
Line 121…..the authors may want to justify the choice of Andersen’s conceptual model over other models they could have used.
Response: Thank you for your suggestion. We chose the Andersen conceptual model because it provides an understanding of how individuals and environmental factors influence health behaviours. This theoretical framework is widely used in literature reviews on healthcare utilisation. This has been justified in lines 147-150.
For Table 1, I think the year the study was conducted ought to be in separate column by itself. This will enable readers to relate them to implementation of the MDGs and contextualize them.
Responses: We agree with this suggestion and a separate column for the date has been added to Table 1.
I have some questions relating to Fig.1;
Responses: We have modified Figure 1 to reflect the new search strategy. With the new search strategy, only four articles were found to have been conducted outside Asia because the term "Asia" appeared in their abstracts.
Lines 210/211…….please give more meaning to ‘perceptions of poor healthcare support’ and ‘concerns about the reactions of healthcare workers
Response: We agree and have clarified the “perception of poor healthcare support” and the “concerns about the reactions of healthcare workers” (lines 276-291).
Secondly, of the 16 articles, 15 were on HIV and 1 was on Syphilis with nothing on Hepatitis B. In this context, I fail to see how you can make any reasonable pronouncements on Syphilis and Hepatitis B screening uptake. On this basis, I suggest you drop off Syphilis and Hep B and make your work entirely about the uptake of HIV screening than about STDs and appropriately reorient your discussion to that effect.
Response: We agree with your suggestion with respect to the discussion and conclusions and have rewritten these sections with respect to HIV only. However, the new search showed up three papers on syphilis and one on hepatitis B, so we believe it is important to highlight this gap and summarise the limited evidence in the results.
We hope that you will be satisfied with the amendments made. If there are any further issues do not hesitate to get in touch. We would like to thank you again for your time and consideration of our manuscript.
Yours sincerely,
Lucie Sabin (on behalf of all co-authors)
Submitted filename: response_reviewers.docx
Decision Letter 1
PONE-D-23-03027R1A systematic review of barriers and facilitators to antenatal screening for HIV, syphilis or hepatitis B in Asia: perspectives of pregnant women, their relatives and health care providers.PLOS ONE
Dear Dr. Sabin, Thank you for resubmitting your manuscript to PLOS ONE. After careful consideration, we feel that it has merit but does not fully meet PLOS ONE’s publication criteria as it currently stands. The manuscript was sent for further review - an initial reviewer advised minor revisions (not accept) and a third (new) reviewer has indicated major revision. The original second reviewer was not available for re-review. You have the benefit then of three careful reviews. Therefore, we invite you to submit a revised version of the manuscript that addresses the points raised during the review process.
Please submit your revised manuscript by Feb 16 2024 11:59PM. If you will need more time than this to complete your revisions, please reply to this message or contact the journal office at gro.solp@enosolp . When you're ready to submit your revision, log on to https://www.editorialmanager.com/pone/ and select the 'Submissions Needing Revision' folder to locate your manuscript file.
Stephen Michael Graham, FRACP, PhD
Additional Editor Comments:
This submission was reviewed for a second time - and again a decision of Major Revision has been made. If you decide to resubmit, then there will need to be clear evidence that you have addressed all concerns of the reviewers for it to be considered for re-review - and then further review will be required anyway.
1. If the authors have adequately addressed your comments raised in a previous round of review and you feel that this manuscript is now acceptable for publication, you may indicate that here to bypass the “Comments to the Author” section, enter your conflict of interest statement in the “Confidential to Editor” section, and submit your "Accept" recommendation.
Reviewer #2: (No Response)
Reviewer #3: (No Response)
2. Is the manuscript technically sound, and do the data support the conclusions?
Reviewer #2: Partly
Reviewer #3: Yes
3. Has the statistical analysis been performed appropriately and rigorously?
4. Have the authors made all data underlying the findings in their manuscript fully available?
Reviewer #3: No
5. Is the manuscript presented in an intelligible fashion and written in standard English?
6. Review Comments to the Author
Reviewer #2: Comments on manuscript PONE-D-23-03027R1
I am grateful to the authors for incorporating the previous comments made. The manuscript looks more refined now but will still need to be improved in some aspects as listed below.
After they have worked on these comments, I believe the work can be accepted for publication
• Line 21………I am wondering if Antenatal screening alone is enough for PMTCT. Shouldn’t it be accompanied by treatment?
• Line 26…..read it again and rectify the grammatical error there….similar error in Line 30/31
• Line 27……..what you sought for in those published articles should be in this line.
• There is nothing about “barriers” in the Results section. If there is, it needs to be made more explicit
• Line 73/74……can the authors show proof that there is a low uptake of STDs screening?
• Who or which persons conducted the initial search? (show with initials)
• Who is the third reviewer?
• Line 133……what is the use of the boldened Error statement there?
• In SPIDER, you defined SAMPLE to include women of childbearing age. I reckoned this work was about Antenatal Screening of Pregnant women. Please clarify the need to include women of childbearing age.
• Review the Data Extraction section for some grammatical omissions and errors. Line 150 is missing “of”. Line 151 …..’categorizes’ instead of ‘categories’.
• Line 160……’that’ instead of ‘who’
Line 321…..rephrase to read “…….allow conclusions to be drawn effectively about HIV alone”
Line 340/341…….there is free screening of HIV, Hep B and Syphilis in many parts of sub-Saharan Africa already.
Line 348……On heterogeneity……there were 19 quantitative studies and you could have evaluated heterogeneity statistically to enable you make a more refined pronouncement on the subject
The Conclusion can be better written…..with emphasis on what specifically needs to be done and by which organization or department or health agency
Reviewer #3: GENERAL COMMENTS:
This review deals with an important topic that could be very useful in the prevention of HIV, syphilis and hepatitis B and transmission of these infections to infants. However, there are several major limitations to the quality of the review which hinder its relevance and applicability. The initial most striking feature of this review is that all four authors are affiliated with only one institute and this institute is in a high-income country that is not in Asia (used as general term here as the authors do not define Asia in their manuscript). Do any of these authors have lived experience of ANC, or healthy policy or practice in the region they are reviewing? If so, it would be helpful to have this information somewhere. Furthermore, the review only includes manuscripts published in English, a major limitation given the region being considered. there are excellent research Institutes throughout Asia, and no doubt this review would be enhanced if it included some collaborations within Asia to increase available grey literature and other studies that may not have been in their search methods.
DETAILED COMMENTS:
“Despite improvements” is vague, some time reference of stats would be helpful here.
STIs is more commonly used now, rather than STDs.
“Antenatal screening” (Sabin, p. 1)
• and treatment. without treatment, screening won’t prevent transmission.
Methods paragraph. typo ‘conducted’ included twice in 1st and last sentence.
What is the definition of ‘Asia’? This should be included in the abstract.
Results section: please define in predisposing characteristics, enabling factors and need factors who you are referring to. The pregnant woman? The health worker?
INTRODUCTION:
“antenatal screening” (Sabin, p. 12) Line 62. And treatment, screening alone will not prevent transmission.
“infected women may transmit infections to their sexual partners or children” (Sabin, p. 13) Line 71. Please rephrase. Women are often infected by their partner, only saying women may give it to their partners overemphasizes their responsibility. What do you mean by infecting their children? Do you mean by MTCT? If so please be specific.
“Meanwhile, it encourages the participation of women living with HIV” (Sabin, p. 13) Line 86. prevention of MTCT of HIV, syphilis and hepatitis B is a shared responsibility, men and communities should also be encouraged to participate.
Preventing male transmission to women during sex, as well as preventing community transmission, of HIV, Syphilis and Hep B is also an effective method of preventing neonatal and infant infections. Whilst I recognise this is not the focus of the review, it should at least be mentioned to prevent misunderstandings and reduce stigma. Overly focusing on pregnant women being the source of transmission to their infants misses an opportunity to emphasise that they are not always the original source of the infection and may not have been able to negotiate appropriate protection for themselves in order to avoid infection.
“An estimated 10,000 new HIV infections occurred 56 among children aged 0–14 years in the Asia Pacific region in 2017” (Sabin, p. 12) Line 56/57. What is the number of infants infected with HIV due to MTCT? You mentioned 10,000 children infected between 0 and 14 years, but clearly not all of these are necessarily due to MTCT.
Line 122, word repetition.
Research type. Why were the articles limited to English? Given most countries in Asia have a primary language other than English this seems a big problem / barrier to identifying relevant research.
Table 3. It would be helpful to also have a column of disease studied in this table.
Line 208. Whose knowledge are you referring to?
Paragraph re male partner’s opinion. In some countries mentioned it may be impossible for a woman to be screened without the express permission of the husband. It would be useful to contrast findings against legal framework for relevant countries as the approach to overcoming this barrier would be very different.
DISCUSSION:
Line 317. Given this review was limited to the English language I do not agree with it being referred to as a “comprehensive synthesis.”
Terminology used is not consistent regarding if this is a scoping review, narrative review or systematic review.
Paragraph 2. Part of the justification for this review was that findings in Asia may differ from that already published in sub-Saharan Africa. Given this, it would be interesting to understand the similarities and differences in more detail in this paragraph.
Line 330/331. Can you reference other differences in ANC screening or barriers that may support this statement?
Line 336/337. It is likely that training programs already exist, could you please highlight what efforts are already made in these settings before suggesting interventions. Again line 340/341 calls for free screening, this would be more helpful if information regarding whether this does or does not exist in the areas included in studies would be more meaningful.
The limitations paragraph needs to mention the limitation of including only English language and the apparent lack of inclusion of experts from the region.
CONCLUSION:
“and STDs” (Sabin, p. 30) Line 454. Please rephrase, you do not address all sexually transmitted infections.
“systematic review” (Sabin, p. 30) Line 354. Be consistent with use of terms narrative or systematic review.
In terms of translating these findings into practice it would be helpful, if possible, to comment in the conclusion as to which factors appeared to be the largest barriers. It may be that this varies in different countries, or at the sub district level. In addition to reviewing studies that look at implementing screening (and treatment), it would be more helpful to also know/contrast this with which countries have policies for ANC screening and treatment and if this is meant to be free or fee for service.
7. PLOS authors have the option to publish the peer review history of their article ( what does this mean? ). If published, this will include your full peer review and any attached files.
Submitted filename: Review of PONE-D-23-03027_R1.docx
Author response to Decision Letter 1
21 Feb 2024
Decision Letter 2
22 Feb 2024
PONE-D-23-03027R2A systematic review of barriers and facilitators to antenatal screening for HIV, syphilis or hepatitis B in Asia: perspectives of pregnant women, their relatives and health care providers.PLOS ONE Dear Dr. Sabin, Thank you for resubmitting your manuscript to PLOS ONE. After careful consideration, we feel that you have addressed comments and suggestions of previous reviewers. I request that you consider comments below about clarity on age ranges and representativeness of the populations studied - if possible.
Please submit your revised manuscript by Apr 07 2024 11:59PM. If you will need more time than this to complete your revisions, please reply to this message or contact the journal office at gro.solp@enosolp . When you're ready to submit your revision, log on to https://www.editorialmanager.com/pone/ and select the 'Submissions Needing Revision' folder to locate your manuscript file.
- A brief letter that responds to the recent point raised by the academic editor. You should upload this letter as a separate file labeled 'Response to Reviewers'.
Journal Requirements:
Please review your reference list to ensure that it is complete and correct. If you have cited papers that have been retracted, please include the rationale for doing so in the manuscript text, or remove these references and replace them with relevant current references. Any changes to the reference list should be mentioned in the rebuttal letter that accompanies your revised manuscript. If you need to cite a retracted article, indicate the article’s retracted status in the References list and also include a citation and full reference for the retraction notice.
Thanks for resubmitting and addressing the comments of the reviewers so comprehensively.
I support publication - however, would it be possible to improve the reporting of these populations by age groups that they represent? Is that something that could be added in a specific column in Table for each study: age range OR what proportion were adolescent pregnancy for example.
Adolescent pregnancy is still common in the region and a very vulnerable population with known poorer outcomes for mother and baby. V neglected population and as at risk for such infections as other pregnant women but perhaps even less likely to be screened? There is a data gap.
If this is not possible, it may still be worth a comment in discussion to highlight lack of data by age, especially in this vulnerable group. a suggested ref for this would be Sabet F, et al. The forgotten girls: .....Lancet. 2023;402:1580-1596.
For journal use only: PONEDEC3
Author response to Decision Letter 2
29 Feb 2024
Dear Dr Graham,
We thank you and the reviewer for your time and comments provided on our manuscript PLONE-D-23-03027 entitled " A systematic review of barriers and facilitators to antenatal screening for HIV, syphilis or hepatitis B in Asia: perspectives of pregnant women, their relatives and health care providers", and we thank you for the opportunity to address these comments. After consideration of your comments, we have made several improvements.
Response: The list of references has been examined. It is complete and correct, and no changes were required.
Response: Thank you for highlighting the importance of this research gap. Unfortunately, it was not possible to report the proportion of adolescent pregnancies in each study, as this information was not always included in the articles. However, we have added a paragraph in the discussion section on the lack of age-specific data, particularly for this vulnerable group of pregnant women, and the importance of filling this data gap (lines 388 to 394).
Decision Letter 3
A systematic review of barriers and facilitators to antenatal screening for HIV, syphilis or hepatitis B in Asia: perspectives of pregnant women, their relatives and health care providers.
PONE-D-23-03027R3
Dear Dr Sabin,
We’re pleased to inform you that your manuscript has been judged scientifically suitable for publication and will be formally accepted for publication once it meets all outstanding technical requirements.
Within one week, you’ll receive an e-mail detailing the required amendments. When these have been addressed, you’ll receive a formal acceptance letter and your manuscript will be scheduled for publication.
An invoice for payment will follow shortly after the formal acceptance. To ensure an efficient process, please log into Editorial Manager at http://www.editorialmanager.com/pone/ , click the 'Update My Information' link at the top of the page, and double check that your user information is up-to-date. If you have any billing related questions, please contact our Author Billing department directly at gro.solp@gnillibrohtua .
If your institution or institutions have a press office, please notify them about your upcoming paper to help maximize its impact. If they’ll be preparing press materials, please inform our press team as soon as possible -- no later than 48 hours after receiving the formal acceptance. Your manuscript will remain under strict press embargo until 2 pm Eastern Time on the date of publication. For more information, please contact gro.solp@sserpeno .
Additional Editor Comments (optional):
Acceptance letter
10 May 2024
I'm pleased to inform you that your manuscript has been deemed suitable for publication in PLOS ONE. Congratulations! Your manuscript is now being handed over to our production team.
At this stage, our production department will prepare your paper for publication. This includes ensuring the following:
* All references, tables, and figures are properly cited
* All relevant supporting information is included in the manuscript submission,
* There are no issues that prevent the paper from being properly typeset
If revisions are needed, the production department will contact you directly to resolve them. If no revisions are needed, you will receive an email when the publication date has been set. At this time, we do not offer pre-publication proofs to authors during production of the accepted work. Please keep in mind that we are working through a large volume of accepted articles, so please give us a few weeks to review your paper and let you know the next and final steps.
Lastly, if your institution or institutions have a press office, please let them know about your upcoming paper now to help maximize its impact. If they'll be preparing press materials, please inform our press team within the next 48 hours. Your manuscript will remain under strict press embargo until 2 pm Eastern Time on the date of publication. For more information, please contact gro.solp@sserpeno .
If we can help with anything else, please email us at gro.solp@eracremotsuc .
Thank you for submitting your work to PLOS ONE and supporting open access.
PLOS ONE Editorial Office Staff
on behalf of
Dr. Stephen Michael Graham

IMAGES
VIDEO
COMMENTS
APA Abstract Format. The abstract page is the second page of your report, right after the title page. This page is numbered 2 on your report. On the first line of the page, center the word Abstract in bold. (Do not underline, italicize, or otherwise format the title.) On the second line, start your abstract.
Here are the steps we recommend when writing abstracts for literature reviews: Introduce the research topic: Begin by stating the subject of your literature review. Explain its significance and relevance in your field. Provide context that highlights the broader impact and necessity of your review. For example, "This literature review focuses ...
A literature review abstract must also provide information on the design of the work, the procedures used, data analysis, etc. The method section helps the reader understand how the work was done. It enlightens the reader about the strategies used to answer the research questions posed. A literature review abstract is incomplete without this ...
This abstract provides an overview of your research questions, problems, or hypotheses, research methods, study results, conclusions, recommendations, and implications. Literature review abstracts in APA style are common in scholarly journals, offering readers a glimpse into the content of the paper. While the maximum word count for an APA ...
This is why the literature review as a research method is more relevant than ever. Traditional literature reviews often lack thoroughness and rigor and are conducted ad hoc, rather than following a specific methodology. Therefore, questions can be raised about the quality and trustworthiness of these types of reviews.
Writing a Literature Review. A literature review is a document or section of a document that collects key sources on a topic and discusses those sources in conversation with each other (also called synthesis). The lit review is an important genre in many disciplines, not just literature (i.e., the study of works of literature such as novels and ...
Limit your abstract to 250 words. 1. Abstract Content . The abstract addresses the following (usually 1-2 sentences per topic): • key aspects of the literature review • problem under investigation or research question(s) • clearly stated hypothesis or hypotheses • methods used (including brief descriptions of the study design, sample ...
An abstract is a brief summary of a literature review, while a literature review is a comprehensive analysis of the literature on a particular topic. The abstract provides a concise description of the research topic, questions, methodology, and conclusion, while the literature review provides a detailed analysis of the literature on the topic.
Examples of literature reviews. Step 1 - Search for relevant literature. Step 2 - Evaluate and select sources. Step 3 - Identify themes, debates, and gaps. Step 4 - Outline your literature review's structure. Step 5 - Write your literature review.
An abstract should give the reader enough detail to determine if the information in the article meets their research needs...and it should make them want to read more! While an abstract is usually anywhere between 150 - 300 words, it is important to always establish with your teacher the desired length of the abstract you are submitting.
The actual review generally has 5 components: Abstract - An abstract is a summary of your literature review. It is made up of the following parts: A contextual sentence about your motivation behind your research topic. Your thesis statement. A descriptive statement about the types of literature used in the review. Summarize your findings.
Step 2: Methods. Next, indicate the research methods that you used to answer your question. This part should be a straightforward description of what you did in one or two sentences. It is usually written in the past simple tense, as it refers to completed actions.
The best proposals are timely and clearly explain why readers should pay attention to the proposed topic. It is not enough for a review to be a summary of the latest growth in the literature: the ...
An abstract of a report of an empirical study should describe: (1) the problem under investigation (2) the participants with specific characteristics such as age, sex, ethnic group (3) essential features of the study method (4) basic findings (5) conclusions and implications or applications. An abstract for a literature review or meta-analysis should describe: (1) the problem or relations ...
Your report, in addition to detailing the methods, results, etc. of your research, should show how your work relates to others' work. A literature review for a research report is often a revision of the review for a research proposal, which can be a revision of a stand-alone review. Each revision should be a fairly extensive revision.
When searching the literature for pertinent papers and reviews, the usual rules apply: be thorough, use different keywords and database sources (e.g., DBLP, Google Scholar, ISI Proceedings, JSTOR Search, Medline, Scopus, Web of Science), and. look at who has cited past relevant papers and book chapters.
1. Outline and identify the purpose of a literature review. As a first step on how to write a literature review, you must know what the research question or topic is and what shape you want your literature review to take. Ensure you understand the research topic inside out, or else seek clarifications.
A literature review may consist of simply a summary of key sources, but in the social sciences, a literature review usually has an organizational pattern and combines both summary and synthesis, often within specific conceptual categories.A summary is a recap of the important information of the source, but a synthesis is a re-organization, or a reshuffling, of that information in a way that ...
Abstract. Literature reviews establish the foundation of academic inquires. However, in the planning field, we lack rigorous systematic reviews. In this article, through a systematic search on the methodology of literature review, we categorize a typology of literature reviews, discuss steps in conducting a systematic literature review, and ...
Ultimately, an abstract is often a factor in determining whether someone will access a manuscript, attend a conference presentation, or consider an application for funding in full. 3 Researchers undertaking systematic searching and screening for a literature review will use the abstract to determine the relevance of the publication for the ...
Background: There is a small body of research on improving the clarity of abstracts in general that is relevant to improving the clarity of abstracts of systematic reviews. Objectives: To summarize this earlier research and indicate its implications for writing the abstracts of systematic reviews. Method: Literature review with commentary on ...
at each of these in turn.IntroductionThe first part of any literature review is a way of inviting your read. into the topic and orientating them. A good introduction tells the reader what the review is about - its s. pe—and what you are going to cover. It may also specifically tell you.
The research, the body of current literature, and the particular objectives should all influence the structure of a literature review. It is also critical to remember that creating a literature review is an ongoing process - as one reads and analyzes the literature, one's understanding may change, which could require rearranging the literature ...
Chapter 9 Methods for Literature Reviews
Therefore, this paper provides a Systematic Literature Review (SLR) of deep learning-based text summarization in both types (extractive and abstractive) between 2014 and 2023. To the best of our knowledge, this is the first SLR that offers a comprehensive overview of extractive and abstractive text summarization techniques based on Deep ...
View PDF HTML (experimental) Abstract: Recent technological advancements have enhanced our ability to collect and analyze rich multimodal data (e.g., speech, video, and eye gaze) to better inform learning and training experiences. While previous reviews have focused on parts of the multimodal pipeline (e.g., conceptual models and data fusion), a comprehensive literature review on the methods ...
Response: On the basis of all the reviewers' comments, we decided to carry out a systematic analysis of the literature rather than a scoping review, using a second person to screen and review articles in duplicate and by searching other databases. We adapted the objectives to those of a systematic literature review (lines 113-115).